Prescribed Minimum Benefits (PMB) is a set of defined benefits to ensure that all medical scheme members have access to certain minimum health services, regardless of the benefit option they have selected. The aim is to provide people with continuous care to improve their health and well-being and to make healthcare more affordable.
In the last few months many allegations have been made that schemes are in fact not all complying with legislation in this regard.
PMBs are a feature of the Medical Schemes Act, in terms of which medical schemes have to cover the costs related to the diagnosis, treatment and care of:
- any emergency medical condition;
- a limited set of 270 medical conditions (defined in the Diagnosis Treatment Pairs);
- and- 25 chronic conditions (defined in the Chronic Disease List).
When deciding whether a condition is a PMB, the doctor should only look at the symptoms and not at any other factors, such as how the injury or condition was contracted. This approach is called diagnosis-based. Once the diagnosis has been made, the appropriate treatment and care is decided upon as well as where the patient should receive the treatment (at a hospital, as an outpatient or at a doctor's rooms).
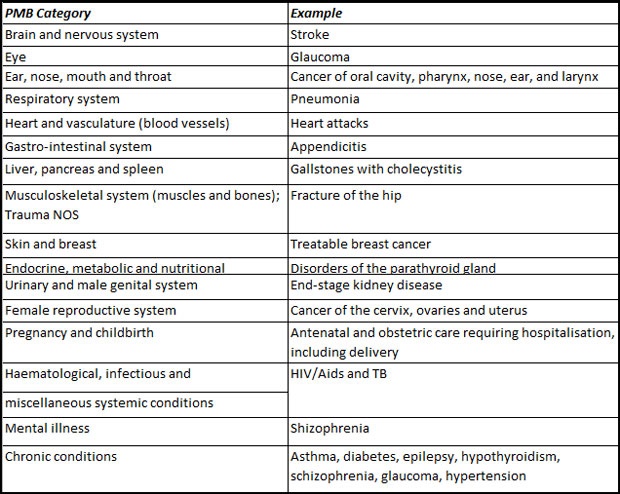
The 270 conditions that qualify for PMB cover are diagnosis-specific and include a range of ailments that can be divided into 15 broad categories:
Click here for a PMB list for all conditions
Know the exclusions
Medical schemes often have a list of conditions – such as cosmetic surgery – for which they will not pay, or circumstances – such as travel costs and examinations for insurance purposes – under which a member has no cover. These are called exclusions.
Exclusions, however, do not apply to PMBs. If you contract septicaemia after cosmetic surgery, for example, your scheme has to provide healthcare cover for the septicaemia part because septicaemia is a PMB. (Cosmetic surgery remains an exclusion.) PMBs are concerned about the diagnosis; it doesn’t matter how you got the condition.
Chronic conditions
To manage risk and ensure appropriate standards of healthcare, so-called treatment algorithms were developed for the CDL conditions.
The algorithms, which have been published in the Government Gazette, can be regarded as benchmarks, or minimum standards, for treatment. This means that the treatment your medical scheme must provide for may not be inferior to the algorithms.
If you have one of the 25 listed chronic diseases, your medical scheme not only has to cover medication, but also doctors’ consultations and tests related to your condition. The scheme may make use of protocols, formularies (lists of specified medicines) and Designated Service Providers (DSPs) to manage this benefit.
Where to get help
PMBs can be a rather complicated subject and your medical scheme might not be able to answer all your questions. Sometimes, your medical scheme may be reluctant to provide you with the cover you are entitled to for a PMB condition and you need someone to champion your cause.
Do not despair. The Council for Medical Schemes (CMS) was established to supervise medical schemes in South Africa. In this role, its first priority is to protect the rights of consumers and to ensure that they are treated fairly.
Therefore, if you have a problem with your medical scheme, contact the CMS in any of the following ways:
Tel: 012 431-0500 / 0861 123 267
Fax: 012 430-7644
E-mail: support@medicalschemes.com
Mail: Private Bag X34, Hatfield, 0028




 Publications
Publications
 Partners
Partners