Tuberculosis (TB) caused by Mycobacterium tuberculosis bacteria, affects about one third (more than 12 million) of all people worldwide. In South Africa, the World Health Organization says TB has reached epidemic proportions.
This chronic infectious disease, explains Dr Andries W Dreyer, Pathologist at the National Institute for Communicable Diseases’ Centre for Tuberculosis, usually manifests in the lungs (pulmonary TB).
Millions of bacteria
TB is spread mainly through the air via droplets (aerosols) when infectious people talk, laugh, spit, sneeze or cough.
“People nearby may inhale the sprayed droplets that contain millions of bacteria and become infected. It only takes one to ten bacteria to establish TB infection,” remarks Dr Dreyer.
TB bacteria have stealthy ways of hiding inside human cells, sidestepping both antibiotics and the body’s immune system and thereby acquiring resistance against TB drugs.
Read: What is tuberculosis?
There is treatment for TB, but it can be complex and last for up to nine months. Dr Dreyer says people with active TB disease are usually treated with several anti-TB drugs, taking daily oral doses for six months.
“Using multiple drugs to treat TB is more effective in killing all the bacteria and avoiding the development of drug-resistant forms like Multidrug-Resistant TB (MDR-TB) and Extensively Drug Resistant TB (XDR-TB),” he explains.
Treating these resistant forms of TB is much more difficult; they don’t respond to treatment with the usual TB drugs. Doctors then have to resort to less effective medications that often cause severe side effects.
Read: What is the cause of tuberculosis?
Most commonly used TB drugs (known as first-line drugs) are Isoniazid (INH) and Rifampin (RIF). They are also combined in a specific treatment regimen with other drugs such as Pyrazinamide (PZN), Ethambutol (EMB) and Streptomycin (STR).
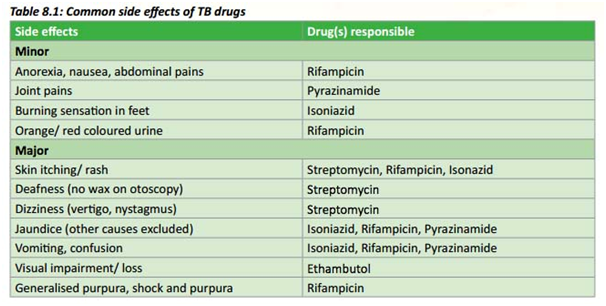
Side effects of TB drugs
TB drugs unfortunately have side effects, some more serious than others. Irene Labuschagne, Dietitian at Stellenbosch University’s Nutrition Information Centre (NICUS), is mostly concerned about gastrointestinal side effects such as nausea, vomiting and weight loss due to decreased appetite, although a dry mouth and sore throat are also often reported.
Source: National Tuberculosis Management Guidelines 2014, Department of Health, RSA
She says acute infectious illnesses such as TB are "accompanied by many complex changes in the metabolism of vital macronutrients such as protein, carbohydrate and fats".
Impact on nutritional status
The body’s response to TB infection – and changes such as high losses of protein – may cause muscle wasting and malabsorption due to due to diarrhoea, loss of fluids, electrolytes and other nutritional reserves.
“All these impair the body’s resistance against TB and have a profound impact on nutritional status,” Labuschagne comments, adding there’s good evidence that being underweight in itself is a "risk factor for the development of tuberculosis in infected persons."
Read: How can tuberculosis prevented?
It’s a vicious cycle, and weight loss, malnutrition and decreased appetite are consequences of the disease, but the most common side effects of essential TB drugs are nausea, vomiting and appetite loss.
So what’s the solution? “TB patients often have a poor appetite, so diet alone is unlikely to able to meet increased requirements for essential vitamins and minerals. That’s why it’s important that TB patients should take a good multivitamin and mineral supplement,” Labuschagne stresses.
Also ask your doctor when is the best time to take your TB medication, as research by the European Lung Foundation suggests that eating food just before taking a TB drug could reduce the medicine’s effectiveness.
Read: How is tuberculosis treated?
How to strengthen your immune system, limit nausea and prevent weight loss
NICUS Dietitian Irene Labuschagne offers these tips:
Nausea and vomiting
- Eat small, frequent meals
- Eat cooled food at room temperature
- Eat dry, salty crackers, pretzels, biscuits and cookies
- Eat light, low-fat foods (rice, scrambled eggs, toast, noodles, bananas, mashed potatoes and custards)
- Drink at least 6-8 glasses of water and liquid daily
- Avoid fatty and fried foods, creamy soups, sweet desserts and milk products
- Don’t lie down immediately after eating.
Constipation
- Add fibre like whole grains, bran and dried fruit (i.e. prunes)
- Fibre-enriched supplements/ bulking agents may be helpful
- Consume extra fluids
- Try to exercise regularly
Avoid processed and refined foods as well as gas-forming foods and beverages (e.g. beer, peas, lentils, cabbage, cauliflower, broccoli, onion, nuts, bran, cucumber, beans and garlic).
Diarrhoea
- Prevent dehydration – replace fluids by drinking plenty of water/rehydration drinks after every loose stool.
- (Make your own oral rehydration fluid at home – combine one litre of cooled cooked water with eight teaspoons of sugar and 1/2 teaspoon of table salt).
- If milk/milk products cause cramps, abdominal discomfort or diarrhoea, switch to a diet low in fat and dairy.
- Focus on soluble fibre foods (fruit, oats and legumes).
- Replenish sodium (salt) and potassium – consume bananas, potatoes, fish, meat and apricot/tomato juice.
- Avoid fried foods (e.g. fried chicken, bacon, French fries and onion rings)and gas-forming foods and drinks.
- Limit fructose (fruit sugar) – avoid soft drinks, pear juice, grapes, honey, dates, figs and nuts.
- Avoid alcohol and caffeine that may dehydrate you further.
Decreased appetite
- Eat 5-6 smaller meals more often instead of three main meals.
- Reduce or cut down on low energy- and nutrient dense foods/beverages.
Note: South African government
healthcare facilities offer a National Therapeutic Programme (NTP) for TB
patients (called the Nutrition Therapeutic Programme in the Western Cape)
providing
combinations of high energy, micronutrient dense porridge, high energy drinks
and therapeutic foods. These are given to adults with communicable
diseases that fall below identified cut-off points in body mass index
(BMI), infants and young children with growth faltering as well
as pregnant and lactating women.
Read more:
World first: child-friendly tuberculosis treatment will be available from 2016
Childhood drug-resistant TB rife in Cape Town
Sources:
1. Dr AW Dreyer, Pathologist (Clinical Microbiologist) Centre for Tuberculosis – National Institute for Communicable Diseases
2. http://www.sciencedaily.com/releases/2014/09/140907084949.htm
3. http://www.sciencedaily.com/releases/2015/06/150602130414.htm
4. Irene Labuschagne Dietitian, NICUS University of Stellenbosch – Faculty of Medicine and Health Sciences




 Publications
Publications
 Partners
Partners