Even though fungal skin infections can be unpleasant and unsightly, they are rarely anything to worry about.
Different fungi cause different types of infections, with different symptoms. These symptoms include redness and itchiness, which are seldom a reason for concern. A bout of athlete’s foot (tinea pedis) can usually be treated with an over-the-counter ointment from the pharmacist without any problem.
While this is reassuring, it doesn’t mean that a fungal infection can’t get out of control. Fungus can also affect the rest of the body, for instance when it enters the lungs – where it can be fatal.
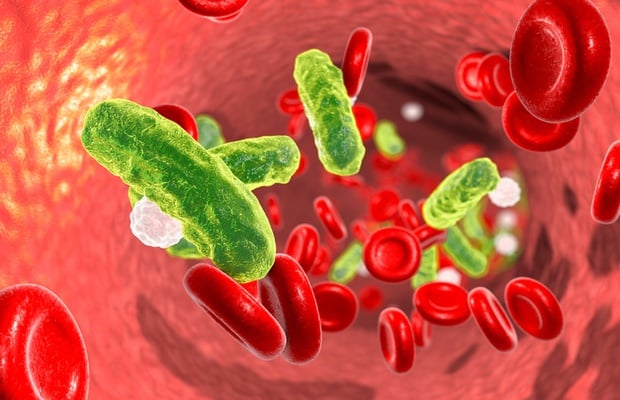
Sepsis is a dangerous condition where a topical skin infection can end up in the bloodstream.
What is sepsis?
But how can a fungal skin infection cause death? This can happen when the infection enters the blood and tissue. The condition is called septicaemia or sepsis and can be fatal if not treated in time.
This dangerous condition is the body’s response to a systematic infection of the blood – symptoms include fever, a fast heartbeat and rapid breathing. When sepsis gets severe, organ failure can take place, causing death.
Sepsis happens when an infection of the skin enters the bloodstream through the lungs, abdomen or urinary tract.
According to research published in the journal Clinical Infectious Diseases, Candida is the fungal strain that is often associated with the onset of sepsis.
Dangerous, more resistant fungus
Besides sepsis, some other fungal infections are currently becoming more resilient to treatment. In 2017, it was reported that nearly three dozen people in the United States had been diagnosed with a deadly antibiotic drug-resistant fungal infection from a strain called Candida auris. When this fungus enters the bloodstream it is extremely resistant to any form of treatment.
And as antibiotic resistance becomes more widespread, especially in hospitals, there is concern that even more fungal spores could turn resistant, according to an article published in the Journal of Clinical Microbiology.
The concern about this specific strain is that it's spreadable via shared surfaces – which makes it a concern in healthcare settings such as hospitals. People who are hospitalised for longer periods of time are especially prone to this resistant fungal strain, especially if their immunity is compromised.
Other deadly fungi
It's not just Candida auris that could escalate into a serious medical problem. There are other common types of fungal spores that can also cause serious disease.
Aspergillus, which can cause aspergillosis – a fungal spore that often affects those with a lung disease or impaired immune system.
Histoplasma – When the spores enter the lungs, it can cause an illness called histoplasmosis among those with an impaired immune system.
Pneumocystic jiroveci can cause serious illness in people with impaired immune systems, especially those who are HIV positive.
How do I control a fungal skin infection?
- Use a topical antifungal cream. In cases where the fungal skin infection doesn’t clear up, a doctor can prescribe a course of antibiotics.
- Keep an eye on any lesions or broken skin – keep this clean to avoid secondary infection.
- Keep shared surfaces, such as bathrooms, clean.
- Always wear clean, dry clothes and shoes.
- Wash your hands to avoid the infection from spreading.
- See a doctor when the infection doesn’t clear up after the first round of treatment, or if you experience any symptoms such as a fever or chills.
Image credits: iStock




 Publications
Publications
 Partners
Partners











