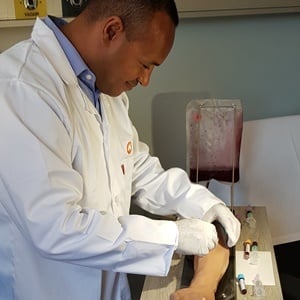
The University of Cape Town (UCT) and Groote Schuur Hospital, in partnership with medical technology company BD, recently launched their simulation ward.
The ward, situated in the New Groote Schuur Hospital Building, is a dedicated space where medical students will simulate real-life emergency situations and be confronted with various aspects which could affect their patients, their colleagues and themselves.
The practical skills
Dr Rachel Weiss, Head of the UCT Clinical Skills Centre, said that despite students going through the academic process and passing their written exams when they’re in an exam venue, these competencies don’t necessarily translate to the clinical environment.
“We know this because we have feedback mechanisms in place. For example, needle stick injury statistics show our students learn the right things but end up doing the wrong things. So, we know that technical knowledge – knowledge and skills – does not necessarily translate into safer clinical practice.
“Therefore, we teach skills that range from phlebotomy (the procedure where blood is taken from a patient) right through to resuscitation, and we use state of the art simulation equipment and methods to do this. Occasionally, we even use simulated patients to do this,” said Weiss.
Many people think that students only start working “practically” when they’re well into their medical degrees and starting their internships at hospitals around the country, but Weiss said that students will now be exposed to the safety simulation ward from their second year.
Honing every skill
“Communication forms a big part of safety. In the second year, we start with communication simulations with ‘patient partners’, so they can learn to communicate as healthcare practitioners, how to examine patients and even how to wash their hands. There is a tutorial given by the nursing staff who specialise in infection control on how to wash hands.
“In the third year, we start with the procedural skills and they learn how to put up intravenous drips, how to catheterise a patient, and so on, but they learn on manikins.
“As they go through the curriculum, it gets more complicated. By the time they reach the sixth year, they need to do an entire simulation, like the resuscitation simulation. In that type of simulation, there is communication, there is needle safety, there are procedures, there is an examination, there is knowing the equipment and that’s how we build this entire process,” said Weiss.
Which steps could be taken to improve the state of South Africa's health system? Share your thoughts by emailing healthnews@health24.com and we may publish your story. Should you wish to remain anonymous, please let us know.
Image credit: Health24




 Publications
Publications
 Partners
Partners










