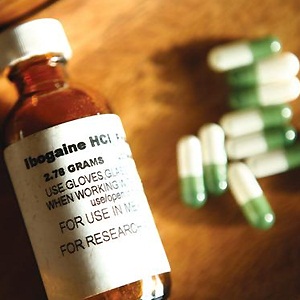
While ibogaine, an active ingredient of the root bark of the African shrub Tabernanthe iboga, was being ignored by the medical establishment in South Africa, pharmacist Charles Rossouw set up an ibogaine treatment clinic in Pretoria.
"I started it and took the plunge and costs to prove its efficacy, although not through scientific means. The proof lies in the tasting, and I see people who were lost walking around drug-free these days," he told Health24.
How it is done
Before treatment begins, a consultation and a number of tests are conducted. "I make certain medical tests compulsory before anyone is accepted for treatment. A medical doctor must also interpret the results of, for instance, the ECG graphs, for me and state that the person is acceptable for treatment," Rossouw says.
The treatment is usually conducted in a darkened room. After he tests for an allergic reaction, Rossouw administers the required dose of ibogaine in capsule form.
According to a review article on ibogaine by Dr Kenneth R. Alper, associate professor of psychiatry and neurology at the New York University School of Medicine, most people will vomit within the first few hours of administration. Ataxia (difficulty with movement and coordination) is also a common symptom.
The review article divides the effects of ibogaine into three phases:
- Acute – This phase starts within one to three hours, and may last for anything from four to eight hours. People typically experience "a panoramic readout of long-term memory" and "visions” or “waking dream” states."
- Evaluative – This phase typically starts between four to eight hours after ingestion, and may last for eight to 20 hours. "The emotional tone of this phase is generally described as neutral and reflective. Attention is still focused on inner subjective experience rather than the external."
- Residual stimulation – Starting after anything from 12 to 24 hours after ingestion, this phase usually lasts for more than three days. The intensity of the subjective psychoactive experience lessens in this period, as the person slowly returns to normal. Trouble sleeping is often reported in this time.
In the period after such a treatment, addicts usually receive intense counselling. An ibogaine treatment seems to provide a break from withdrawal symptoms, and a temporary reduction in the need to take the drug that the person is addicted to. Thus, there is something of a window period in which the psychological side of the addiction can be attended to.
But how well does it really work?
As Gerbus Muller, a toxicologist at the University of Stellenbosch, points out, "There is scant objective information on clinical efficacy, and clinical reports in scientific medical journals only cover a few dozen patients."
Furthermore, administering ibogaine is illegal in the United States and the drug has not yet been registered in South Africa. "My e-mails and enquiries two years ago to authorities went unanswered. The substance is not listed anywhere, and I am using it as a herbal/natural product, which is legal," Rossouw says.
Thus, ibogaine seems to inhabit a space on the frontiers of science – it may turn out to be effective, and alternatively, it may turn out to be very dangerous. The kind of randomised clinical studies in humans that can give definitive answers to these questions has, however, not yet been done.
Nevertheless, ibogaine is not a new drug, and a substantial amount of research has been done on it.
What the research says
The most compelling scientific evidence for the use of ibogaine against drug addiction stems from animal studies. As long ago as 1991, studies found that ibogaine helped to diminish opioid self-administration in rats and to alleviate withdrawal symptoms.
Unfortunately, very few studies have been done in human subjects, and when they were done, they were done outside of traditional clinical settings. Yet, research conducted by Dr Deborah Mash, Professor of Neurology at the University of Miami, indicates that the use of the drug to treat opioid dependence in humans may be viable. Yet, until further trials, serious concerns about the safety and efficacy of ibogain will remain.
"Serious toxic effects (in therapeutic doses) include: slowing of the heart, fall in blood pressure, heart failure, seizures, paralysis, and respiratory arrest (these toxic effects have been reported following therapy with ibogaine)," says Muller. Furthermore, "deaths (related to cardiac arrhythmia) have been reported in several individuals taking ibogaine. (There is, however, inadequate data to determine whether ibogaine may have been a primary factor in these cases.)"
Another concern is that ibogaine may cause brain damage. One study has, however, suggested that this may only be a risk at doses higher than those required for therapeutic purposes.
There is no solid information on the long-term effects of using ibogaine.
And, despite extensive research, the exact mechanism of the drug is still not fully understood. "Ibogaine appears to have a novel mechanism of action that differs from other existing pharmacotherapies of addiction," Alper writes. "Ibogaine’s effects may result from complex interactions between multiple neurotransmitter systems rather than predominant activity within a single neurotransmitter system."
A medical subculture
In the early 1990s the US Food and Drug Administration gave its approval for an ibogaine study in humans. Due to a lack of funds, this study never took place. The US National Institute on Drug Abuse (NIDA) decided not to support such a study at a meeting in 1995.
With the kind of scientific studies that would give more clarity on the safety and efficacy of ibogaine not happening, the underground movement, or what Alper calls a "medical subculture" related to ibogaine, gained momentum.
In a telephone interview, Alper describes Charles Rossouw as a typical exponent of this subculture.
This may help to explain the lack of recognition ibogaine has received from the scientific establishment. Other contributing factors to this situation may be the drug's roots in the West African Bwiti religion and the use of the drug for what Rossouw calls "spiritual reasons".
Furthermore, Alper suggests that the best way to learn about the drug is to witness the treatment and to speak to someone who has undergone a treatment.
He points out that, even though there are safety concerns, it is also not safe to be a heroin addict. Thus, people with a serious heroin or cocaine addiction may be willing to take the risk, despite the lack of scientific evidence.
It is also important that when someone does decide to take ibogaine, it is done under experienced supervision. Without a formal medical network to refer to, determining the expertise of the person conducting the treatment may, however, be difficult.
The future for ibogaine
According to Rossouw, the demand for treatment has surged dramatically since Carte Blanche aired a programme on ibogaine. And, according to Alper, the ibogaine subculture is also growing very fast internationally.
Nevertheless, the studies needed to answer the crucial questions about the safety and efficacy of the drug in humans are yet to be conducted. And, until they are, ibogaine will remain shrouded in uncertainty.
Ibogaine research continues to suffer from a serious lack of funding. According to Alper's review article, "Ibogaine is particularly unattractive to industry for several reasons: its mechanism of action is apparently complex and incompletely understood, it may present significant safety issues, it is a naturally occurring alkaloid whose structure cannot itself be patented, and some of its use patents are close to expiration."
"Two clinical trials were, however, recently funded - one at the University of Miami, Florida and one at the Beer Yaakov Mental Health Centre, in Tel Aviv," Muller said.
Even so, clarity on the crucial questions regarding ibogaine still seems some way off.
Visit our Substance abuse Centre for more information on addiction.




 Publications
Publications
 Partners
Partners









