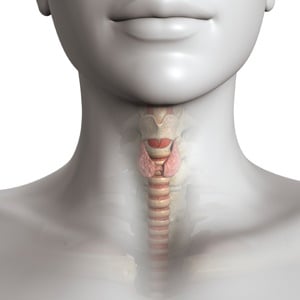
But, what is the thyroid gland?
The thyroid gland is a small, butterfly-shaped gland in your neck, and mostly, it just gets on with its job of governing your body’s metabolism, in collaboration with your hypothalamus and your pituitary gland, both located in your brain and known as your endocrine system.
The challenge is that this system doesn’t get the same attention as, for instance, your circulatory system or the digestive system which display obvious symptoms when something goes wrong.
Ever heard of irritable bowel syndrome? When you’re faced with extreme and recurrent abdominal pains and diarrhoea you know something is wrong.
Read: What your thyroid does for your body
The 411 on thyroid disease
There are different types of thyroid dysfunctions: (i) Hypothyroidism, (ii) Hyperthyroidism, and (iii) malignant thyroids.
Hypothyroidism – The slug
Hypothyroidism is where the thyroid gland is under-functioning (sluggish). It is caused by a variety of things, including autoimmune disease, treatment for hyperthyroidism, thyroid surgery, radiation therapy, and some medications. Less frequently, it could be caused by congenital disease, a pituitary disorder, pregnancy, or an iodine deficiency.
What are the symptoms?
The symptoms of an under functioning thyroid (Hypothyroidism) are a little less obvious, and are easily confused with the results of stress, or other lifestyle diseases. They include fatigue, weakness, weight gain, elevated cholesterol, hair loss or coarse, dry hair, muscle cramps, and an intolerance for cold conditions.
If hypothyroidism isn’t treated, it becomes worse – and you maybe become forgetful, your thought processes may be slow, or you may be depressed. It could also lead to heart problems, mental health issues, and nerve damage (called peripheral neuropathy), as well as infertility among women, and birth defects among children.
Untreated, it could lead to a condition known as myxedema, which is rare, but life-threatening, as it includes low blood pressure, decreased breathing, decreased body temperature, unresponsiveness and even a coma.
Image: Signs and symptoms of hypothyroidism. Häggström, Mikael. "Medical gallery of Mikael Häggström 2014". Wikiversity Journal of Medicine 1 (2). DOI:10.15347/wjm/2014.008. ISSN 20018762. - Own work. Reference: Longo, DL; Fauci, AS; Kasper, DL; Hauser, SL; Jameson, JL; Loscalzo, J (2011) "341: disorders of the thyroid gland" in Harrison's principles of internal medicine. (18th ed.), New York City: McGraw-Hill ISBN: 007174889X.
Hyperthyroidism – The over-zealous
Hyperthyroidism is where the thyroid gland is over-functioning (over active). This condition sees the body producing excess hormones, which then impact on how the rest of your body functions.
There are different types of hyperthyroidism, falling under diagnoses Graves’ disease, hyper functioning thyroid nodules, and thyroiditis.
Hyperthyroidism tends to run in families, and it tends to be more common among women than among men.
What are the symptoms?
Symptoms of an over-functioning thyroid, or hyperthyroidism, are a little easier to detect, and include fatigue, hand tremors, mood swings, anxiety, rapid heartbeat, heart palpitations, dry skin and insomnia, and even sudden weight loss.
Left untreated, it could lead to heart problems, brittle bones, poor eye sight, red swollen skin, and even thyrotoxic crisis, which includes a rapid pulse, fever, and even delirium. It’s clear that this needs to be treated immediately, with ongoing care required once diagnosis has been made.
Read: Thyroid-related diseases may vary by race
Get tested to avoid more serious conditions
It’s easy to see how hypothyroidism can be confused with many other illnesses that affect South African men and women, but it is imperative that you work with your doctor to identify links between symptoms.
All it takes is a simple blood test that will provide diagnosis. Treatment for hypothyroidism is non-invasive and affordable – and essential to quality of life.
It is particularly important for women of childbearing age to understand the implications of hypothyroidism, as it can severely impact the development of unborn children.
If undiagnosed during pregnancy and immediately after birth, children affected by hypothyroidism do not develop (mentally or physically) as they should, occasionally leading to catastrophic outcomes.
What are these catastrophic outcomes?
Hypothyroidism can affect both mother and baby. For the baby, the need for assisted birth (whether this be a C-section or the use of forceps) is greater. Hypothyroidism also affects a baby’s IQ and results in developmental delays.
With regards to mums, hypothyroidism often results in: more bleeding, a higher risk of postpartum depression, and, may impact a mother’s ability to breast feed, i.e. she may find it difficult to “let down”.
It has also been shown to increase perinatal morbidity and mortality. For instance, mums with hypothyroidism generally suffer with more complications during and post birth.
Read: Advanced image scans spotting more thyroid cancer
The heel-prick test on the baby – what could that show and what would the treatment be?
The test itself is a heel-prick for infants that should ideally be done at birth, on every child. The heel prick test is standard in developed countries, and identifies with complete certainty whether a baby has an underactive thyroid.
Research has shown that 1 in 3000/4000 live births results in a diagnosis of hypothyroidism.
This means that it is inevitable that these babies will be mentally challenged.
Of course, there are social and financial implications to consider, such as a financial dependence on the State and the need for community support where babies have special needs.
Thyroxine, which is inexpensive and easily available is the medicine used to prevent the dangerous consequences of an underactive thyroid and will in 100% of cases prevent these complications
It is true that endocrinologists, the specialist doctors that treat thyroid disease, are in short supply in South Africa.
However, specialist doctors at Chris Hani Baragwanath Academic Hospital are pioneering a scanning protocol and training programme that, if rolled out to primary care clinics across the country, with the assistance of corporates like Merck, a global pharmaceutical Company with headquarters in Germany, will make testing and diagnosis of thyroid disease much quicker and easier.
Read: Thyroid disorders tied to complications in pregnancy
What would the scanning protocol entail?
At Chris Hani Baragwanath Hospital, we have been fortunate to recently (in November 2015) receive an ultrasound system donated by Merck.
This allows our team of endocrinologists to widely screen patients for Goitres, multi-nodular Goitres or nodules.
We can also perform Fine needle aspiration(FNA) to evaluate whether a cancer is present or not, with ultrasound guidance.
In essence, the ultrasound system enables us to diagnose thyroid malignancies straight away.
The protocol goes further though, in a single visit, patients can be screened, have the disease identified and begin treatment.
It has reduced the time taken to diagnose and treat thyroid malignancies from 3-6 months to 7-10 days. The traditional approach requiring the involvement of various specialities, including nuclear medicine, surgeons, cytologists and endocrinologists.
Now, using multimedia technology all these departments work in concert to save patients time, anxiety and improve treatment outcomes.
Image: Chris Hani Baragwanath Hospital staff receive an ultrasound system in November 2015 donated by Merck
What is the general treatment for people with thyroid disorders, and how expensive is it?
Treatment (as discussed earlier) is widely available both in the Private and Public sectors. The medicines available are inexpensive, and the advantage of Thyroxine, is that it is available in multiple doses (for example, 25mg, 50mg, or 100mg). The tablets are also scored so it is easily broken, which ensures tighter titrations.
How often should a person who has hypothyroidism, for instance, be tested?
It is vitally important that once diagnosis of an underactive thyroid is made, a patient has follow up blood tests done every six weeks until their TSH is within a normal range.
Once the patient has stable thyroid functions, a blood test need only be done once or twice a year.
For women, puberty, pregnancy and perimenopause are stages when greater fluctuations are expected. This often requires fine tuning of their thyroid medications.
This is quite expensive, on top of the medication, in the private sector – why is it affordable at Bara?
While it is relatively expensive to manage the condition within the Private healthcare system, secondary and tertiary state institutions are more than capable of managing thyroid disease. As a hospital, we have also embarked on empowering primary healthcare services to manage the disease better. We regularly hold training symposiums for doctors, with the financial grants we’ve received from Merck
In additions, we will be implementing an IT system that will allow telemedicine in the field of thyroidology.
Do you have any stats on how many people live with thyroid disease in SA, and how many are possibly undiagnosed?
There are no South African statistics on the disease (which is why greater awareness if necessary), although if you look at international literature the prevalence (while it varies with age and gender) varies from 4% to 10% amongst the elderly.
Having said this, our team, with the sponsorship received by Merck, will be embarking on a project to establish the prevalence of both hypothyroidism and hyperthyroidism in the SA.
With regard to thyroid malignancy, no statistics are available, although prevalence of malignancy across the world has increased. With our new protocol and the donated ultrasound we have managed to diagnose 20 cases of thyroid malignancy in the last 5 months.
What diseases have similar symptoms as hypothyroidism and could be confused with it?
The symptoms of thyroid disease are non-specific and can be confused with anaemia, depression and other causes of weight gain to name a few.
Thyroid hormone self-tests are available from pharmacies such as Clicks, but apparently they don’t do a full-spectrum test. The test could show that you don’t have thyroid problems, but that’s maybe because it doesn’t test all the hormones, please can you comment on this?
A self-test focusses on TSH so it points you in the direction of an underactive thyroid, but it does not give you an absolute value for T4 and antibody status. It also misses pituitary causes of hypothyroidism, albeit rare.
Read more:
Childhood abuse may lead to thyroid problems
Understanding thyroid stimulating hormone - TSH




 Publications
Publications
 Partners
Partners
















