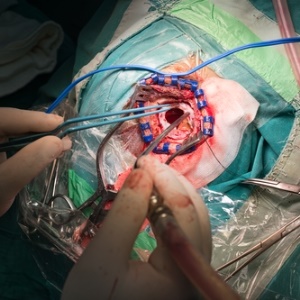
A craniotomy literally means "a hole in the skull". The procedure is used to gain access to the brain for neurosurgical operations.
Why is it done?
Many conditions affecting structures inside the skull need surgery, and craniotomy allows the surgeon access. Some of these conditions are:
- Tumours,
- Trauma,
- Intracerebral bleeds or clots,
- Abnormal blood vessels like aneurysms, or arterio-venous malformations,
- Parkinson' disease,
- Infection like brain abscess,
- Some forms of seizures (epilepsy), and
- Some disorders of the cerebellum.
How is it done?
Craniotomy is usually done under general anaesthesia, but may be done under local anaesthetic in certain cases.
Careful imaging studies (X-rays, scans) must be done beforehand to determine the best place on the skull to site the hole, and how large the hole must be to allow adequate surgical access.
In the operating theatre, the relevant part of the patient's skull is shaved and the incision site is marked out. The scalp is then cleaned with antiseptic solutions and the area draped with sterile towels. The skin is incised in a 5/8ths circle, dissected off the skull, and then flapped back and held out of the way. Bleeding is controlled. A hole is drilled through the skull.
If a large hole is required, a piece of skull is removed and preserved. Once the surgery inside the skull is finished, the "lid" of bone is replaced. If this is very large, it will need to be held in place with tiny wires, metal strips or any other technique favored by the neurosurgeon. Very small holes may be just drilled out and left to reseal themselves under the skin.
The flap of skin is replaced and sutured back in place.
Risks and complications
As with any operation, risks are related to:
- The anaesthesia - breathing problems, and drug reactions,
- Any underlying conditions - like heart problems, some brain tumours or brain swelling may make anaesthesia very difficult,
- Surgery in general - bleeding and infection are the most important,
- Cranial surgery specifically - damage to brain structures, other nerves and blood vessels, all of which can cause muscle weakness or paralysis. Damage to or loss of mental functions such as speech, vision, memory, hearing or understanding can also occur.
Outcome
The overall outcome will depend on the nature of the underlying condition making the craniotomy necessary in the first place.
The craniotomy itself seldom has complications. The scalp has a very rich blood supply, so wounds usually heal quickly and well, with little infection. It may take 812 weeks for the skull bone flap - especially large ones - to become fully reunited with the surrounding skull bone. Pain, swelling and other symptoms in the immediate post-operative period are well controlled with medication, and patients generally have little discomfort once discharged.
(Dr A G Hall)




 Publications
Publications
 Partners
Partners











