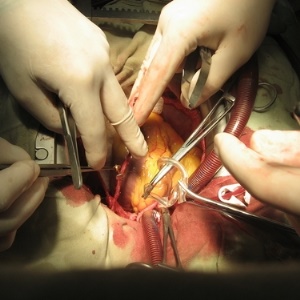
Coronary artery bypass graft, or CABG, is an operation to bypass a diseased or obstructed heart artery. A blood vessel from another part of the patient's body is removed (harvested) and grafted onto the heart to provide oxygenated blood to the heart muscle. The blood vessel harvested is one which can safely be removed without causing problems. Most often, saphenous veins from the lower or upper leg are used. Where possible, the left internal mammary artery ( LIMA) running on the underside of the breastbone is "hijacked" and diverted to supply the heart instead. In some patients, the radial artery of the forearm can be used as a graft.
Why is it done and for whom?
Blockages in the heart's arteries are nearly always due to cholesterol deposits with added blood clot formation. Lesser amounts of blockage may cause angina (chest pain during exertion). Critical or total blockage can cause death of the heart muscle. This is called a heart attack, causing permanent damage to heart muscle.
A person with symptoms suggesting coronary artery disease (CAD) will be investigated by a cardiologist, and an angiogram will indicate the need for treatment. The majority of patients with CAD have related problems as well, such as diabetes or hypertension. For any individual patient, all relevant factors are considered in selecting the best treatment, which may be medical management only, or some form of intervention, such as inserting a stent, or CABG.
Some of the more important factors favouring CABG rather than other forms of treatment are:
- number of arteries - if two or more arteries are involved, CABG is often a better choice;
- anatomy - some parts of some arteries simply cannot be accessed by stenting;
- severity - totally blocked arteries, especially those with heavy calcium deposits can seldom be opened with stents;
- size - smaller arteries have a better chance of staying open with CABG than with stents;
- length - a long section of diseased artery would need too many stents, so CABG is the better choice here; and
- previous failed stents.
Bypass surgery is merely a "plumbing job", and does not cure the underlying problems which led to the blockages in the first place. Unless these are treated, the condition will progress to affect the rest of the heart's arteries, and cause blockages in the vein grafts used for bypasses.
How is it done?
CABG is major surgery, and can be done in several ways. In each method, general anaesthesia is used, veins/arteries are harvested and then grafted onto the heart. The method for this may differ according to the facilities available, the skill and experience of the surgeon, and factors specific to the individual patient. Established techniques of bypass grafting are:
Conventional
Under anaesthesia, veins/arteries are harvested. The patient's chest is opened, and prepared for the surgery. Anti-clotting drugs are administered, and the patient is connected to the heart-lung machine, which takes over the functions of both the heart and the lungs. The patient's heart and respiration are then stopped, giving the surgeon a still heart to work on. Once the grafting is done, the heart and lungs are restarted: their functions and all grafts are carefully checked for problems (like leaks, or abnormal heart rhythms). Anti-clotting drugs are then reversed with antidotes, and the patient is disconnected from the heart-lung machine. The chest is closed with steel wires which are left in place permanently, and the skin wound is sutured. The patient is transferred to the ICU, where he may need to remain on a ventilator for another few hours before the breathing tube is safely removed. Most uncomplicated cases can be discharged 7-10 days after surgery, though the time to full recovery and resumption of normal activities may be up to three months for some.
Off-pump (OPCAB)
Here, under anaesthesia, veins/arteries are harvested and the chest is opened in the usual way. However, in an OPCAB, the patient is not connected to the heart-lung machine, and the heart is not stopped. This is often known as "beating heart surgery". It is technically far more difficult for the surgeon: many compare it to a mechanic trying to repair a car while its engine is running. If complications occur, or the surgeon cannot complete the OPCAB, then the procedure is converted to the conventional style, in which the patient is put on the heart-lung machine to complete the operation.
Successful OPCAB surgery relies heavily on the surgeon's skill and experience, and most heart centres in South Africa do very few such procedures. OPCAB is usually done for patients needing only one bypass graft: doing several grafts would take much longer than the conventional way.
Endoscopic
This is grafting done using a scope (camera) instrument inserted into the chest. Patients' chests are not cut open, nor are they put on the heart-lung machine. The procedure is technically possible, but is very difficult and time-consuming, and thus seldom done.
Outcome
In the hands of an experienced surgeon, the outcome of CABG is generally good.
Important immediate or short-term complications are
- cardiovascular: stroke, heart attack, rhythm disturbances,
- bleeding,
- infection, or
- post-cardiotomy syndrome: chest discomfort with fluid collection in the lungs.
Long-term complications are few, but a serious one is non-healing/infection of the breastbone.
CABG may be repeated if other arteries or the veins grafts become blocked in later years.
(Dr A G Hall)




 Publications
Publications
 Partners
Partners











