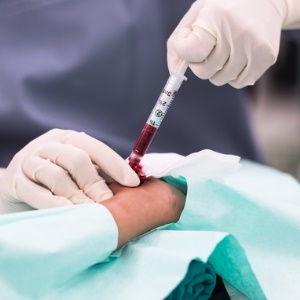
What is it?
An arterial blood gas test is performed by collecting a small amount of arterial blood for analysis in a clinical laboratory.
Alternative names
The test is sometimes just referred to as a "blood gas".
Why is the procedure performed?
Normally, arterial blood is rich in oxygen as it comes from the heart and flows towards the tissues. An arterial blood gas test can be used to evaluate the lung function or the acid-base status of the patient.
Interpretation
The attending physician will evaluate the patient's acid-base status by studying the various measurements. If the pH is increased (above 7.44) the patient is alkalotic and if it is decreased (below 7.36) the patient is acidotic.
The next step is to decide if the condition is caused by the respiratory system (lungs) or a metabolic problem (mainly kidney). The pCO 2 (partial pressure of carbon dioxide) indicates respiratory function and the HCO 3 (bicarbonate) indicates metabolic function. If the pCO 2 is increased it suggests a respiratory acidosis and if decreased a respiratory alkalosis. An increased HCO 3 fits in with a metabolic alkalosis and a decreased HCO 3 fits in with a metabolic acidosis.
An example:
pH 7,19 (7,36 - 7,44)
pCO 2 3,0 (4,6 - 6,0) kPa
HCO 3 16,0 (24 - 30) mmol/l
pH < than 7,36 - acidosis (Metabolic or respiratory)
pCO 2 < than 4,6 - respiratory alkalosis
HCO 3 < than 24 - metabolic acidosis
The low HCO 3 value (metabolic acidosis) corresponds with the pH. The "respiratory alkalosis" is caused by the patient trying to compensate for the metabolic acidosis. Various diseases can cause a metabolic acidosis including diabetes, intoxication (alcohol, salicylate), kidney failure and acute diarrhoea.
How should I prepare?
As with any medical procedure, it is important that you tell your health care provider about all medical problems that you may have and all medication that you are using. For instance, aspirin interferes with blood clotting, causing the site where blood was taken from to require a longer period of compression. Try to relax and breathe normally, as hyperventilation might influence the result.
How is the procedure performed?
The procedure is usually performed by a doctor or a registered nurse. The blood sample is taken from an artery, in contrast to usual blood tests which require venous blood. The test is therefore more invasive and there should be a convincing reason why it should be performed.
The most commonly used site for collecting an arterial sample is the radial artery at the wrist - where you would feel your pulse to count your heart rate. A short "butterfly" needle, connected to a thin plastic tube, is inserted into the artery. The blood is collected in a heparinised syringe, because the heparin prevents the blood from clotting. The blood tube should be placed on ice and immediately taken to the laboratory for analysis. It is important for you not to make a fist while the blood is being collected, but to relax your hand.
An arterial blood collection is more painful than regular blood tests, as the artery is positioned deeper in the tissues and the first attempt may not be successful. There are veins running in that area, so if the needle hits a vein and venous blood is sucked into the tube the procedure needs to be repeated. Sometimes a topical anaesthetic is used to avoid pain.
After the needle has been removed the area should be compressed for at least 10 minutes. You will probably get a small bruise at the puncture sight. It is important not to exercise or carry heavy objects for about 24 hours afterwards.
Risks
Problems occur very rarely. In people with clotting problems or those who take drugs such as aspirin, there may be ongoing bleeding. Keep an eye on the puncture sight for a few days and immediately tell your doctor if something worries you.
What are the limitations of the procedure?
If venous blood is collected, the test has to be repeated. If the blood is not taken to the laboratory very soon after collection, the results will not be reliable.




 Publications
Publications
 Partners
Partners















