Hypertension is diagnosed only after several careful measurements show that the systolic and/or diastolic blood pressure (BP) is consistently above normal.
This is because normal BP fluctuates and stressful situations, such as a visit to your doctor’s rooms, can elevate your BP temporarily. The exception to the above rule is if your BP is severely elevated above 180/110mmHg.
Note that, in most cases, a single reading isn’t sufficient and that the effect of “white coat” hypertension may be overestimated. Increasingly, 24-hour BP monitoring is used to diagnose hypertension and obviates the need for repeated measurements. It needs only to be performed once for diagnosis.
In most cases, an extensive work-up isn’t needed to diagnose hypertension.
How blood pressure is measured
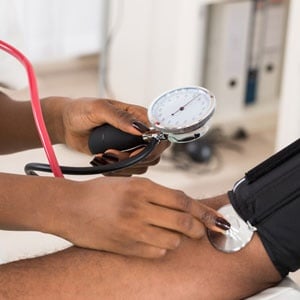
BP is measured using a sphygmomanometer.
It consists of a soft cuff, wrapped around your upper arm, which is then inflated to put pressure on the arm as well as the brachial artery that runs the length of the limb. This is linked to a column of mercury with precisely calibrated numbers. A stethoscope is placed on the inner side of the elbow crease, just below the cuff. This is right above the main artery (the brachial artery) in your arm.
Until a couple of years ago, the manual method was the norm: that is, listening to the heartbeat over the brachial artery on the inside of the upper arm while deflating the cuff and watching the mercury column fall. When the heartbeat became audible, it meant that the pressure just wasn’t high enough to cut off the blood flow in your brachial artery.
The point at which this happened was measured and counted as your systolic pressure. Releasing the pressure even more caused disappearance of the heartbeat. This is the diastolic pressure.
In recent years new, automated BP monitors, which accurately measure BP through electronic signals, have become the new gold standard. Several readings from an automated BP monitor (from a reputable manufacturer with certification) are more reliable than any manual reading. Automated BP monitors are available for use by healthcare professionals, and at home. Devices that measure BP at the wrist aren’t recommended.
Whether BP is measured manually or with an automated machine, it should always be measured in the upper arm in quiet surroundings. The cuff needs to be the correct size and you need to sit with your back supported, your legs uncrossed and on the floor, and your arm supported at heart level. Several readings need to be taken every one to two minutes until readings stabilise.
Initial readings are often higher than later readings, and the mean of the final two readings should be recorded. Have a healthcare provider check your BP annually.
The following tests are performed to diagnose hypertension and related conditions:
1. Routine investigations
Physical examination and medical history confirm the presence of hypertension and determine its severity. It also evaluates possible damage to organs, establishes the presence of associated diseases that increase the risk of complications, and looks for possible causes of secondary hypertension.
Your doctor will look into your eyes with a special instrument to assess possible damage to the retina.
Other tests may include:
- Creatinine and potassium test: This is a blood test that indicates how well the kidneys are functioning and whether they’re damaged.
- Urine analysis: Abnormalities, such as the presence of blood and protein, give an indication of kidney damage and may suggest that the kidneys are also involved in causing secondary hypertension.
- Blood glucose (fasting) and HbA1C: These can indicate the presence of diabetes, which increases the risk of complications.
- Fasting lipogram: This diagnoses high cholesterol, which adds to the risk of complications in an individual with hypertension.
- Electrocardiogram (ECG): This is a recording of the electrical activity of the heart, which indicates the degree of damage to the heart and which detects previous heart attacks.
If there is reason to suspect that BP measurements taken in the doctor's rooms don’t represent true BP (for example, as a result of white coat hypertension), or if there are large fluctuations in BP, out-of-office BP monitoring over 24 hours may be needed. This can take the form of self-monitoring at home or continuous ambulatory BP monitoring.
The 24-hour monitor is now considered a highly accurate and reproducible investigation, and predicts outcome far more accurately than office BP. A daytime mean blood equivalent to office 140/90mmHg is 135/85mmHg.
2. Special tests to detect organ damage
Other tests may be done to determine if hypertension has caused damage to your heart or kidneys, or if you’ve had a stroke.
- Chest X-ray: This shows the size of the heart and presence of fluid in the lungs.
- Echocardiogram: This shows a live image of the heart and its contractions on a television screen.
- CAT or MRI scans: Computerised axial tomography (CAT) or magnetic resonance imaging (MRI) can show damaged brain tissue in a person who has had a stroke.
3. Tests to detect causes of secondary hypertension
Tests that may be done to check for causes of possible secondary hypertension, such as kidney artery problems (renovascular disease) or hormonal (endocrine) problems, include:
- Renal and duplex Doppler ultrasound: A test that uses sound waves to detect narrowing of the arteries that supply blood to the kidneys and signs of kidney disease.
- CT or direct renal artery angiogram: Dye is injected and its course followed through the renal arteries to show any narrowing in the arteries.
- Plasma renin activity and aldosterone determination: A blood test that determines the level of renin and aldosterone – hormones that play an important role in BP control.
- NMA and norepinephrine test: The levels of these two hormones are high in certain rare tumours of the adrenal glands that result in hypertension.
- Sleep studies to detect sleep apnoea.
Reviewed by Prof Brian Rayner, nephrologist and Director of the Hypertension Clinic, Groote Schuur Hospital. MBChB, FCP, MMed, PhD. May 2018.




 Publications
Publications
 Partners
Partners















