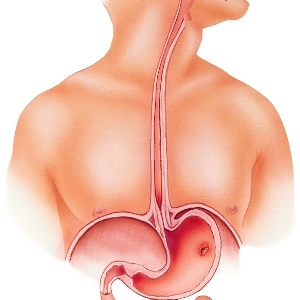
Your doctor may suspect a peptic ulcer when he or she notes your symptoms, but because the symptoms of the different ulcers are very alike, several tests may be ordered to make a specific diagnosis.
Before embarking on extensive testing, doctors usually scrutinise an individual’s medical and family history as well as his/her current lifestyle. Questions about eating habits, smoking and drinking, and use of any other medication, especially non-steroidal anti-inflammatories (NSAIDs), may be asked.
Acid-blocking medication may be prescribed for four weeks as an initial treatment. Many ulcers may heal within this period of time. If not, further testing may be needed.
Gastroscopy
For diagnosing a peptic ulcer, your doctor will most likely first request an upper gastrointestinal endoscopy or gastroscopy – the preferred diagnostic test. Note that if your doctor has requested a gastroscopy, you’ll need to fast for 12 hours before the procedure.
During the gastroscopy, you’ll be sedated and a slim, flexible, lighted tube (a scope) will be inserted through your mouth to examine your oesophagus, duodenum and stomach. The doctor can also take a biopsy of the lining of the stomach tissue to test for H. pylori infection during the procedure.
Biopsies, especially of stomach or gastric ulcers that may be cancerous, can be examined under a microscope to determine if cancer is present.
Barium X-rays
For diagnosing a stomach ulcer, your doctor may request a barium X-ray of your upper gastrointestinal tract. This isn’t uncomfortable and involves no risk.
You swallow barium, a white chalky substance that’s visible on X-ray (it’s sometimes called a "barium milkshake"), and will be asked to lie down on a tilted examining table. The tilting distributes the barium evenly around your upper digestive tract so that the X-ray can capture images at different angles. This allows the doctor to locate the ulcer, and to determine its type and severity.
Note, however, that this isn’t a very accurate procedure: in almost 20% of cases, the X-rays don’t detect ulcers.
Blood and stool tests
The doctor may also order a blood test to check for anaemia (which indicates internal bleeding), request an analysis of a stool sample to check for blood (indicating a bleeding ulcer), or do other blood tests to check for the presence of active H. pylori bacteria.
A breath, urine, saliva or stool test can also be used diagnose H. pylori.
Differential diagnosis
Dyspepsia, or discomfort and pain in the upper abdomen, is the most common symptom related to peptic ulcers, but is seen in other conditions, too.
These conditions include:
- Oesophagitis
- Gastritis
- Pancreatitis
- Pericarditis
- Heart attack
- Gallstones
- Gastro-oesophageal reflux disease (GORD)
- Crohn’s disease
- Hepatitis
- Stomach cancer
The above conditions need to be ruled out before a peptic-ulcer diagnosis can be made.
Read more:
What are peptic ulcers?
The causes of peptic ulcers
The complications of peptic ulcers
Reviewed by Dr Estelle Wilken, senior specialist in Internal Medicine and Gastroenterology at Tygerberg Hospital. December 2017.




 Publications
Publications
 Partners
Partners