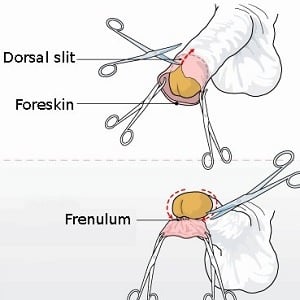
Circumcision, which has been subject of fierce debate, involves cutting the foreskin around the tip of the penis.
Several studies conducted in Africa indicated that circumcision could help reduce the spread of HIV, the virus that causes AIDS.
The overall risk of adverse events associated with male circumcision is low, with minor bleeding and inflammation cited as the most common complication
| How a foreskin increases HIV risk |
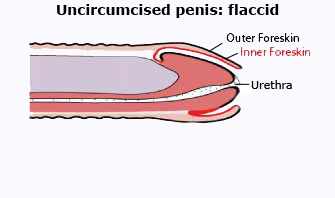 |
The outer foreskin and the penis shaft are covered by a fairly thick layer of skin, which provides a protective barrier against HIV. The inner foreskin is covered by only a very thin mucous membrane, allowing HIV easy access. red line indicates inner foreskin |
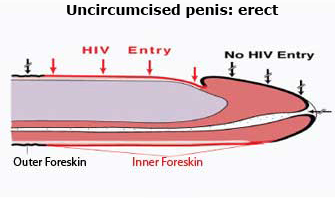 |
During heterosexual intercourse, the foreskin is pulled back down the penis shaft. This exposes the inner foreskin to vaginal secretions, and serves as a large area where HIV transmission could take place. red line indicates inner foreskin |
| Adapted from McCoombe & Short, 2006 |
Circumcision: the kindest cut
One of the most effective weapons against HIV/Aids is in fact 4 300 years old. Circumcision has become a hot topic in the field of HIV prevention.
Image: Isaac's circumcision, Regensburg c1300.jpg. Source: WikiMedia Commons
The results of three recent studies on male circumcision provide strong evidence that this simple surgery could save millions of lives.
Robert Bailey, Professor of Epidemiology at the University of Ilinois at Chicago, speaking at the 2007 International Aids Society Conference on HIV Pathogenises, Treatment and Prevention, said that male circumcision has been likened to a vaccine.
"Not a perfect vaccine, but an effective one - about 60% effective in preventing new HIV infections in adult heterosexual men," said Bailey.
Oldest surgery in the world
Bailey pointed out that circumcision is hardly a new health-related intervention: the ancient Egyptians performed the procedure over 4 300 years ago, and it developed independently in several different cultures around the world.
It is likely the oldest and most common surgery ever performed.
Today, about 30 - 35% of men are circumcised. When performed under antiseptic conditions by a trained practitioner, said Bailey, it is a simple, low-risk procedure.
Trials stopped because so effective
The most persuasive evidence to date of circumcision's efficacy in reducing HIV infection has come from three randomised controlled trials conducted in South Africa, Uganda and Kenya.
The trials were all stopped before going to full completion. Bailey explained: "This was because the protective effect of circumcision was so strong there was miniscule statistical doubt it was effective, and it wouldn't have been ethical to continue to withhold the procedure from uncircumcised men in the trials."
The trials showed a reduction of HIV incidence in circumcised men of 57%. "One would be challenged to find any public health intervention with such a strong and consistent efficacy. Certainly, we have nothing else like this in the field of HIV prevention," said Bailey.
In the light of the trial results, the World Health Organization (WHO) and the United Nations Programme on HIV/Aids (UNAIDS) issued a joint statement in which they strongly endorse male circumcision as a means of HIV prevention, asserting that its efficacy "has been proven beyond reasonable doubt" and that it "should be considered as part of a comprehensive HIV prevention package."
Not just HIV
In addition to HIV, circumcision offers protection against several other conditions, said Bailey, including urinary tract infections in baby boys, and penile cancer, chancroid and human papillomavirus in adult men.
Female sexual partners of circumcised men benefit too, experiencing lower rates of cervical cancer and chlamydia.
6 years, $23 million, 1 million deaths later
Bailey lamented the fact that, even as early as 2000-2001, there was already ample evidence - admittedly from less rigorous studies - that an uncircumcised man was far more likely to be HIV-infected than a circumcised man.
"We've come to the same conclusion that was staring us in the face then," said Bailey. "Six years, 23 million dollars and probably a million new preventable infections later.
"Only a handful of scientists, and no policy makers, were persuaded that circumcision should be considered as a new HIV prevention strategy. Randomised control trials had to be done before the international health community could be persuaded to move.
"It raises the question: have we raised the bar too high for converting evidence to action in the face of a crippling pandemic?
"One can't help but contemplate that if it were a drug or a compound or a shot with a fancy label, international agencies and donors would have been fighting to make it available many months, even years ago.
"But no one stands to profit from male circumcision - except the 4 000 men in Africa who will be newly infected tomorrow, and their partners and children."
Won't circumcised men take more risks?
Concerns have been raised that if circumcision were promoted as preventing HIV, circumcised men may feel protected and take more risks, a phenomenon known as "sexual disinhibition". As an example of this, Bailey quoted one circumcised man as saying: "Ah, I have a natural condom."
Watch: The pros and cons of male circumcision. Source Youtube
However, Bailey reported that data from the three trials suggest that sexual disinhibition did not occur. The level of risk behaviour of both circumcised and uncircumcised men came out about equal; overall risk behaviour and sexually transmitted diseases (STIs) declined for all participants in the trial.
Bailey further pointed out that: "All the highest HIV prevalence countries are those where circumcision is little practised. No country with nearly universal circumcision coverage has ever had an adult HIV prevalence higher than 8%."
He added that, in addition to its high efficacy, circumcision is also cost effective - more so the faster countries act. "The faster we scale up, the more infections we can prevent - and each infection averted costs us less."
Will men agree to get circumcised?
Bailey believes that, if the large numbers of people who came to participate in the trials are anything to go by, then men are highly likely to find circumcision initiatives acceptable.
A circumcision programme should also engage women in its planning, because they, as sex partners and mothers, will be instrumental in encouraging male circumcision. In previous studies on circumcision acceptability, women particularly were in favour of their sons getting circumcised, and felt that circumcised men were cleaner and less likely to be carrying an STI.
Why a foreskin increases risk
The outer surface of the foreskin and the penile shaft are covered by a relatively thick layer, which provides a protective barrier against HIV.
By contrast, the inner mucosal layer of the foreskin is very thin, and allows HIV and other pathogens easy access to target cells lying near the surface.
During heterosexual intercourse, in an uncircumcised man the foreskin is pulled back down the shaft of the penis, and the whole inner surface of the foreskin is exposed to vaginal secretions, providing a large area where HIV transmission could take place.
Additional information source for this article:
Szabo, R and Short, RV. How does male circumcision protect against HIV infection? British Medical Journal, 2000;320:1592-1594
Related article:
Male circumcision - you still need a condom
A-Z of circumcision




 Publications
Publications
 Partners
Partners