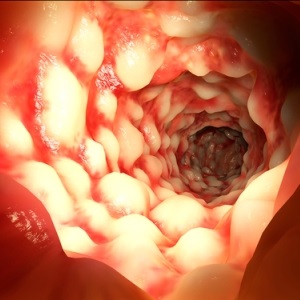
Proctitis is inflammation of the lining of the rectum, called the rectal mucosa. Proctitis can be short term (acute) or long term (chronic). Proctitis has many causes. It may be a side effect of medical treatments like radiation therapy or antibiotics. Sexually transmitted diseases like gonorrhea, herpes, and chlamydia may also cause proctitis. Inflammation of the rectal mucosa may be related to ulcerative colitis or Crohn's disease, autoimmune conditions that cause inflammation in the colon or small intestine. Other causes include rectal injury, bacterial infection, allergies, and malfunction of the nerves in the rectum.
The most common symptom is a frequent or continuous sensation or urge to have a bowel movement. Other symptoms include constipation, a feeling of rectal fullness, left-sided abdominal pain, passage of mucus through the rectum, rectal bleeding, and anorectal pain.
Physicians diagnose proctitis by looking inside the rectum with a proctoscope or a sigmoidoscope. A biopsy (a tiny piece of tissue from the rectum) may be removed and tested for diseases or infections. A stool sample may also reveal infecting bacteria. If the physician suspects Crohn's disease or ulcerative colitis, colonoscopy or barium enema x rays may be used to examine areas of the intestine.
Treatment depends on the cause of proctitis. For example, the physician may prescribe antibiotics for proctitis caused by bacterial infection. If the inflammation is caused by Crohn's disease or ulcerative colitis, the physician may recommend the drug 5-aminosalicyclic acid (5ASA) or corticosteroids applied directly to the area in enema or suppository form, or taken orally in pill form. Enema and suppository applications are usually more effective, but some patients may require a combination of oral and rectal applications. - (February 2009)
Source: National Digestive Disease Information Clearinghouse (NDDIC)




 Publications
Publications
 Partners
Partners














