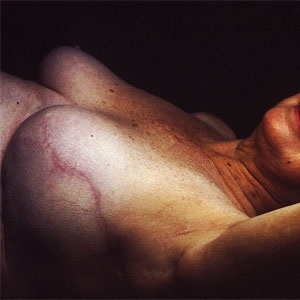
Breast augmentation is a plastic surgery term for breast enlargement surgery.
This can be done with implant insertion or fat grafting surgery. Here fat is removed from other body areas that can be cosmetically enhanced through liposuction and then this fat is injected into the breast to increase the size and projection.
In terms of breast cancer patients, implant reconstruction or reconstruction with own tissue is used to rebuild a breast after mastectomy.
Read: Types of mastectomy
Breast reconstruction surgery is done to correct defects after the removal of cancerous tissue.
Being diagnosed with any form of cancer is emotional and traumatic, and when the treatment involves removing parts of your body it can be even more so.
Women who lose breasts to cancer have a long road of fighting the disease ahead of them and it’s important for them to find the emotional strength needed to face this challenge.
Professor Frank Graewe, head of plastic surgery at Tygerberg Academic Hospital says that breast reconstruction plays an important part in building emotional resilience.
What you need to be considered however before the decision to have breast reconstruction is made
- The best time to have breast reconstruction is during your mastectomy. Although not essential, the results and psychological well-being tend to be better when breast reconstruction is done at the same time as the mastectomy during one operation.
- It’s important to note that the sensations in your breast will no longer be the same. There won’t be feeling in the nipple for example.
- Having a reconstruction does mean that recovery will be longer so it will take longer to return to normal activities – although I believe the longer term benefits far outweigh the initial inconvenience.
- If you have a very active job or are an athlete then it’s important to consider how your motion will be affected once you have fully recovered. Down time is less after implant reconstruction compared to reconstruction with abdominal perforator flaps for example.
On the other hand studies have shown that the patient satisfaction rate is higher in the long run with own tissue reconstructions than with implant reconstructions.
Read: Breast reconstruction after mastectomy: yes or no?
And then there are various types of reconstructions available:
- Implants: a salt water or silicone implant is inserted (possibly the more well-known of the options).
- ‘Flap’ reconstruction: in this case tissue is transplanted from another part of your body (like your stomach, thigh or back).
There are pros and cons
Very simply, implant reconstructions are easier to perform and have less recovery time but long term they might be prone to problems.
‘Flap’ surgery does take longer to recover from but they have better long term results.
And in the case of ‘perforator flap’ surgery – a relatively new and ground-breaking procedure – the invasiveness of the surgery is limited as muscle tissue is not used. It’s important to ask your plastic surgeon to carefully outline all the options.
As breast reconstruction is a major operation it’s important to make sure you know the risks and what the recovery will entail.
Questions to ask your plastic surgeon, breast cancer surgeon and oncologist:
· What is the ideal timing for my reconstruction in relation to my other treatments?
· How long will the surgery take?
· Is there anything I can do prepare for the surgery
· What anaesthesia will I need?
· How much discomfort or pain will I feel?
· Will you insert drains? And, will I need help caring for these at home?
· How long will I need to be in hospital for?
· How long is my recovery likely to be at home?
· What will and won’t be possible after the surgery? Will I need help at home?
Surgery is more than likely going to be your first line of attack against your cancer, so it is worthwhile considering, while undergoing that surgery, to have your breast or breasts reconstructed.
It’s difficult to tell how someone will react emotionally to having a breast removed as it’s a part of the body inextricably linked to being a woman. And we believe that the emotional strength gained from feeling ‘whole’ is a vital part of a woman’s fight against her cancer.
About the author, Frank Graewe
In 2014 Professor Frank Graewe was an integral part of the team that performed the world’s first successful penile transplant. Prof Graewe was responsible for all the microsurgery during the harvesting as well as the re-attachment.
This is a highlight in a career specialising in microsurgery, craniofacial surgery, and cosmetic breast surgery and breast reconstructions. He is currently the Head of the Plastic Surgery Division at Stellenbosch University as well as the Head of the Craniofacial Unit at Tygerberg Academic Hospital and works closely together with related specialties such as neurosurgery and maxillofacial surgery.
In addition to his participation in the ground breaking penile transplant, Prof Graewe has also invented and published a new innovative surgical procedure for infants with severe midface hypoplasia, which is is a minimally invasive technique of midface distraction without osteotomies.
Prof Graewe is actively involved in CSI initiatives that translate into the improvement of life quality and are specifically topical to the South African landscape. These include the World Craniofacial Foundation, the Smile Foundation South Africa and We Love Africa.




 Publications
Publications
 Partners
Partners