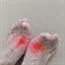
Gout is a metabolic disorder that may be inherited. It is characterized by recurrent acute joint inflammation (gouty arthritis) usually in the extremities, caused by crystals that are deposited in and around the joints. These crystals come from blood that contains markedly high concentrations of uric acid (urate), a waste product of digestion that is normally excreted in the urine.
Symptoms include heat, red and shiny skin, and extreme tenderness and pain in the affected joints. It tends to affect the peripheral joints, most often those in the big toe, but can also affect the knees, elbows, thumbs or fingers.
The arthritis may become chronic and cause joint deformity. Tophi – small, hard lumps of urate deposits – may also form around the ankles, hands, tips of the elbows and earlobes. The tophi may erupt, causing a discharge.
Collection of urate crystals in the kidneys can lead to kidney stones.
Not all persons with high urate levels in their blood (hyperuricaemia) develop gout, but the greater the degree and duration of hyperuricaemia, the greater the risk of crystal deposition and acute gout attacks. Gout is a common disease and one of the oldest in medical literature. One of the oldest drugs in therapeutics, colchicine, is used for the acute attack of gout.
Causes
Urate is normally steadily excreted in the urine. In some people the mechanism to excrete the uric acid is defective. These people are known as under-excretors, and constitute the majority of gout sufferers. This is aggravated by certain medications, especially diuretics and kidney disease. It occurs commonly in the setting of people with heart disease, obesity and diabetes and commonly in women who are post-menopausal who use diuretics.
Hyperuricaemia may also be caused by blood conditions such as lymphoma, leukaemia and haemolytic anaemia (where blood cells are destroyed), and by other cancers or psoriasis. In this situation the problem is over-production and the patients are called over-producers.
If urate levels in the blood rise too high (hyperuricaemia) the urate starts to crystallise as needle-like crystals in the joint fluid (synovial fluid) and joint lining (synovial lining). It forms deposits where the temperature is lower, as it is in the extremities, particularly around the big toe.
Some foods may contribute to high blood levels of urate. Marked rises in urate often follow overindulgence in high protein foods, especially if alcoholic beverages are also consumed. In most cases alcohol does not contain uric acid, but further prevents the excretion of uric acid via the kidneys.
Urate can also form small, plate-like crystals in the kidneys, where they may aggregate to form gravel or stones.
Intense joint inflammation occurs when white blood cells engulf the crystals.
In order for this to occur there is often a precipitating event. Known precipitating factors for gout attacks include acute infection, emotional upset, the use of diuretic drugs such as Furosemide or Lasix, surgery and trauma. In fact any “change” in the daily routine of a patient can precipitate an attack. This includes a food or alcohol binge. But even a new (especially high protein) reducing diet can aggravate the onset of an attack.
Symptoms
Acute gouty arthritis
- Sudden onset of intense pain in a joint, typically the big toe, sometimes also the ankle, knee, elbow or wrist.
- The onset can be almost immediate or over minutes to hours.
- Swelling, inflammation and a feeling that the joint is very hot.
- Tense, warm, shiny red or purplish overlying skin.
- Occasionally, in extreme cases, chills and fever.
Although gout is probably inborn, the first attack of gouty arthritis usually does not appear until middle age, mainly in men. The first few attacks may come (often at night) and go without apparent reason, but are often precipitated by the factors above. The symptoms usually settle down within days. With prompt treatment, the pain and inflammation can be brought under control quickly, although attacks can recur if the underlying problem, a high urate level, is not treated. Later untreated attacks may persist for weeks or even become chronic with daily pain.
Chronic joint symptoms
Asymptomatic intervals tend to become shorter as the disease progresses. Attacks start to occur more frequently and may start to develop in more than one joint and in unusual sites including knees, hands and elbows.
- Joints can become permanently deformed as a result of erosion by the crystals, so that hands and feet lose their mobility. In rare cases, the shoulder, chest joints or neck vertebrae may be involved.
Tophi
When gout has been present for a longer period, urate deposits called 'tophi' develop. They appear as small, hard lumps around ankles, hands, the tips of the elbows, earlobes and even around the vocal chords and the spinal chord.
- Eventually they can cause pain or stiffness.
- They can also protrude and finally erupt, causing a discharge of chalky material containing urate crystals.
- Neglected tophi cause damage to the underlying bone and joints and are an absolute indication to treat the underlying condition and not just the symptoms of the attacks.
Prevalence
Gout occurs mainly in middle-aged men, who represent 90 percent of all gout sufferers. Often they are obese and suffer from high blood pressure (hypertension). The remainder are usually post-menopausal women; gout is rare in children.
Course
Generally, because gout is such a painful affliction, people seek help and receive treatment. If the diagnosis is made early, current therapy can permit a normal life. However, if treatment is not followed or urate levels remain high, the disease can eventually cause serious joint afflictions and kidney problems.
For those with advanced disease, it is possible to correct joint structure to a degree. Tophi can be resolved, joint function improved, and kidney problems stopped.
About 10 to 20 percent of gout sufferers develop kidney stones. These may lead to obstruction and infection, which may damage kidney tissue. Many people with gout have high blood pressure. This condition can also damage the kidneys. In these cases, progressive destruction of kidney tissue may lead to further problems with urate excretion, which further raises urate levels.
When gout appears before the age of 30 it tends to be more severe.
Genetic predisposition for an abnormality in handling urate accounts for approximately half of all cases. A family history of gout can be a risk factor.
- Male sex in middle age.
- High blood pressure.
- Drugs: thiazide diuretics, aspirin, tuberculosis medication (pyrazinamide and ethambutol).
- Obesity or excessive weight gain, especially in youth.
- Moderate to heavy alcohol intake.
- Abnormal kidney function.
- A Western lifestyle.
- Underlying diseases with a high turnover of cells (cancers – especially blood cancers and haemolytic anaemia).
Conditions that can trigger gout
- Recent surgery.
- Dehydration.
- Joint injury.
- Excessive dining.
- Heavy alcohol intake.
- Stress.
- Change in diet.
- Foods with a high protein content such as red meat, shell fish, legumes and soya.
When to see a doctor
Call your doctor if:
- Joint pain develops suddenly, especially when there has been no physical injury and if the pain is associated with redness and extreme tenderness.
- Joint pain recurs or lasts more than a few days, especially when associated with chills or fever (rheumatoid arthritis needs to be excluded).
- When, in known gout, symptoms become more severe or side effects of medication (allopurinol or colchicine) occur.
- When any severe colicky back pains develop and radiate into the groin – this may be caused by a kidney stone.
- If you are developing lumps (tophi).
- If attacks are more frequent or if they are affecting different or multiple joints.
- If the attacks are frequent and not settling and / or tophi are developing, consider asking your doctor regarding a specialist.
Preparing for your doctor's visit
It is important that the doctor gets the relevant history of the episode. All medication taken should be known by name and dosage, as some drugs can cause a gout attack. If gout has been present for a while, old X-rays related to the illness may be useful in follow-up.
Diagnosis
You should see a doctor for any kind of joint pain to get an accurate diagnosis.
- The history is important and can lead to a diagnosis by itself. Gout usually presents in one joint at a time, while other arthritic conditions, such as systemic lupus and rheumatoid arthritis, usually involves multiple joints simultaneously.
- A thorough examination can confirm the suspicion of gout.
- Blood tests may support the diagnosis by showing high urate levels, but these levels are also sometimes elevated in the absence of gout. Equally, the uric acid in the blood may be normal in some cases of acute gout. The diagnosis is a clinical one in many cases, made from the history and the examination, and special tests may be normal.
- A definite diagnosis can be made if the needle-shaped urate crystals are found in tissue or joint fluid. A small part of suspected tissue (for example, one of the tophi) is biopsied (removed) under local anaesthetic. Alternatively, a sample of fluid is removed from the affected joint, which can be quite painful, but provides useful information. The material is examined under the microscope to look for crystals. A special polarized light microscopy technique is used to see the crystals.
- X-rays can show punched-out lesions in the bone just underneath the cartilage of the joint, commonly in the joint of the big toe. Tophi may also be seen on X-rays.
Treatment
General
When you seek treatment for an acute gout attack, your doctor’s main treatment objectives will be:
- Termination of the acute attack and relief of pain
- Prevention of recurrent attacks (if they are frequent) by daily prophylactic use of medication
- Prevention of further deposition of urate crystals and resolution of existing tophi (achieved by lowering the urate levels in body fluids)
A preventative maintenance programme should be followed to avert the erosion of bone and joint cartilage, and kidney damage. Underlying obesity, high blood pressure and high cholesterol levels should be controlled.
Home
When you wake up with an acute episode, ibuprofen or any other anti-inflammatory drug in the home pharmacy might help.
- Rest and elevate the inflamed joint to ease some discomfort.
- Ice-pack applications can help reduce pain and decrease inflammation.
- Paracetamol and codeine are not very effective, and aspirin might make the condition worse because it prevents excretion of urate by the kidneys.
- Consult a doctor the next morning or, if the pain is excruciating, go to an emergency department.
- During an acute attack or when under treatment by a doctor, drink fluids abundantly to combat dehydration, increase fluid in the kidneys and dilute urate in the urine.
Medication
In many cases, prompt treatment with appropriate drugs solves the problem permanently. However, since recurring attacks are possible, chronic sufferers may have to remain on low-level drug therapy for extended periods, sometimes for life.
Acute attacks:
- Colchicine: usually a dramatic response to oral colchicine. Joint pain generally begins to subside after 12 hours of treatment and is gone within 36 to 48 hours. Colchicine may have unfavourable interactions with antidepressants, tranquillisers or antihistamines; it is contra-indicated in pregnancy because of the risk of birth defects.
- Nonsteroidal anti-inflammatory drugs: Ibuprofen (Brufen), indomethacin (Indocid), naproxen (Naprosyn), piroxicam and sulindac are effective in acute attacks of established gout. These drugs should be taken with food, as they can erode the lining of the stomach. Of note is that stomach ulcers can develop irrespective of the route of administration of anti-inflammatory drugs. Therefore a stomach ulcer can still develop if an injection or even topical route is used. Care should be taken in elderly people, especially those with kidney problems. Newer drugs called COXIBS can be used especially when there is concern regarding stomach ulcer problems.
- Corticosteroids: this group, which includes prednisone, consists of powerful anti-inflammatory agents that can be used in the treatment of acute gout. The drugs can be administered orally or injected directly into the inflamed joint. Corticosteroids can be prescribed to patients who have accompanying kidney, liver, or gastrointestinal problems. Long-term chronic use of corticosteroids is discouraged because of serious long-term side effects. However, they remain very useful for severe and resistant cases.
Chronic elevated blood urate levels
- Drugs that block urate production: Allopurinol reduces urate formation. It is very useful in the management of repeated episodes of urate kidney stones. However, there is a risk of side-effects that include a rash, liver damage, mild gastrointestinal problems, decreased numbers of white blood cells, drowsiness and disorientation. Allopurinol can interact with other medications, especially anticoagulants and diuretics.
- Absolute compliance is required when taking allopurinol. Erratic use will increase gout attacks. Even stopping for a day might bring on an attack. Once on the drug, it is usually “forever” as stopping the drug will simply restart the cycle of increasing attacks.
- Urinary alkalinisers: Sodium bicarbonate and trisodium citrate can be used with great success to prevent kidney stones. These medications do not treat the actual gout itself.
- A diet with exclusion of high protein containing foods is introduced.
Important: Drugs that lower the urate concentration should only be started after the acute symptoms have settled down completely. If started when the attack is still active, or even if there is mild residual heat in the joint, these medications can worsen an acute attack. If the person is already taking these drugs and has a breakthrough attack, then the advice is to continue the allopurinol. DO NOT STOP IT. Rather treat the attack but maintain the allopurinol. The allopurinol should only be stopped if the attack becomes resistant and will not settle down.
An increased dose of urate-lowering medications can precipitate gout attacks in some people. In these cases, low doses of colchicine or anti-inflammatory can be given to prevent the development of acute gout.
Surgery
Withdrawal of fluid from the affected joint (arthrocentesis) may help, and often corticosteroids can be injected into the joint space at the same time. (In addition, the most reliable way of making an accurate diagnosis is to examine the aspirated fluid under the microscope.)
- Surgical removal of tophi is occasionally done, but can lead to serious secondary infection and generalized sepsis.
- Extracorporal lithotrypsy can help destroy large kidney stones. During this procedure, shock waves are transmitted through the body and focused on the kidney stone. The stone is cracked up into small pieces that can be passed normally in the urine. It might be necessary to remove the stones in an operation if this fails.
Prevention
- Avoid certain protein-rich foods that can lead to decreased urate excretion: organ meats (liver, brains and kidneys), shellfish, fatty fish, asparagus, spinach and most dried beans. Some people find particular foods which affect them as individuals. These should be avoided in that instance.
- Increase your fluid intake – this is very important to decrease the possibility of urate crystal formation in the kidney tracts.
- Avoid alcohol, as it retards elimination of urate.
- If you are obese, control your body weight.
If you are a man and gouty arthritis runs in your family, these preventative measures are particularly important. Blood and urine tests during routine check-ups will alert your doctor to a potential for gout attacks. He or she may prescribe drugs to reduce the body's production of urate and to encourage the excretion of excess urate. It is a treatable disease. Lowering the uric acid level to an acceptable level is paramount.




 Publications
Publications
 Partners
Partners