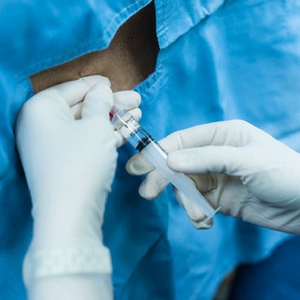
Lack of knowledge and experience are contributing to an inexcusable number of maternal deaths from spinal anaesthesia in South Africa, amounting to an estimated 41% of all anaesthesia-related deaths.
Mari Hudson writes in What's New Doc
Real-life scenario 1
A 16-year-old pregnant girl who never attended an antenatal clinic, is admitted to a level 1 hospital. The two doctors on duty at the obstetric unit are a young, inexperienced community service doctor and a medical officer.
It quickly becomes clear that the mother-to-be needs an emergency Caesarean section. A delay of three hours to reach the referral hospital could result in death for mother and baby, or both. The medical officer and the community service doctor rush off to theatre. Everything goes well until the newborn requires resuscitation. When the community service doctor abandons the mother to attend to the baby, the situation changes dramatically and within minutes the mother dies.
If an experienced and well-trained senior doctor had administered the anaesthetic, the younger doctor could have focused on the resuscitation and the young mother might still be alive today.
Real-life scenario 2
At a level 1 hospital in South Africa a 35-year-old woman has been allowed, shockingly, to be in labour for three days. Then a spinal anaesthetic is unwisely administered. She is septic, on intravenous antibiotics and dyspnoeic. She develops catastrophic hypotension and convulsions immediately following spinal anaesthesia and does not respond to resuscitation.
Spinal anaesthesia should not have been administered to this haemodynamically unstable patient; general anaesthesia should have been chosen instead.
The risks of spinal anaesthesia
“Inexperienced doctors (and some experienced doctors but not in anaesthesia) think that spinal anaesthesia is a technique that anybody who can stick a needle into somebody’s back can safely administer,” says UFS specialist Dr Gillian Lamacraft.
“They don’t take into account that a spinal anaesthetic not only blocks sensory and motor fibres, it also blocks the sympathetic nervous system, resulting in sudden-onset, profound vasodilatation. The block level is usually from about T4 down, so a patient who is dehydrated, intravascularly depleted due to haemorrhage or sepsis, or haemodynamically unstable, experiences a precipitous drop in blood pressure after spinal anaesthesia, which can swiftly result in cardiac arrest.”
Low blood pressure can also cause loss of consciousness, which can result in death from apnoea or aspiration of gastric contents.
This lack of knowledge and experience are contributing to an inexcusable number of maternal deaths from spinal anaesthesia in South Africa, amounting to an estimated 41% of all anaesthesia-related deaths here.
When performed by one of South Africa’s 1 000 specialist anaesthetists, spinal anaesthesia is perfectly safe. It is the inappropriate and incorrect use of spinal anaesthesia, plus the inability to recognise and manage its well-known complications, that is the problem.
General anaesthesia is not the solution either and should be avoided because pregnant women are all oedematous to a varying degree, and it’s ten times more difficult to intubate them. They can also die very rapidly from hypoxia as a result of the physiological changes of pregnancy. Swopping spinal for general anaesthesia could result in an epidemic of maternal deaths from failed intubation.
This is an edited extract of an article first published in What’s New Doc, 2nd issue, March 2009. What’s New Doc is a publication for medical doctors, produced in association with Health24.
Read more:
Anaesthesia shock: fatal decisions
Maternal deaths anaesthesia related
South Africa fails mothers
Anaesthesia related deaths in kids




 Publications
Publications
 Partners
Partners















