Elections are looming and the ANC has promised national health insurance within five years. Will this mean the end of medical aid schemes and private practice as we know it?
JOAN VAN ZYL writes in What’s New Doc
To many, it’s the only answer to the enormous inequalities in South Africa’s healthcare system. Others fear it may limit the variety of health services available in the country. And some warn that it will mean the end of private practice and medical aid schemes.
No wonder we’re all a bit confused about national health insurance (NHI), the ANC’s plan for sorting out the huge divides in the health sector.
NHI is definitely on its way though, that much is clear. It will be a health insurance fund to which everyone with a job will contribute, and from which all South Africans will be able to benefit, whether they contribute or not.
The ultimate aim is to have a system in which the public health service is of such a high standard that everyone will want to use it. This service will be provided free and paid for by the NHI scheme, which will be funded by government, and by citizens according to income.
But the rest of the NHI picture is pretty murky, and surrounded by many questions and fears. Where will the resources be found to make the plan work? What will happen to private healthcare? Will medical schemes disappear? Will doctors have to accept lower incomes? Will former private patients be forced into a system that can only offer limited services?
NHI is not a new idea. It’s been bandied about for more than 15 years, and the reason it’s back in the spotlight is that it’s very prominent in the ANC’s election manifesto.
No doubt it can be a wonderful system – if it works. The problem is the time frame. According to their manifesto, the ANC wants NHI up and running within five years, but critics say this is impossible as the country cannot possibly afford such a system within that time frame, and too much of our health infrastructure has to be repaired first.
Even finance minister Trevor Manuel has expressed doubts about the practical side of the plan. After all, it took Germany more than 120 years to achieve an inclusive health insurance system.
At the recent Sascro/Sasmo oncology conference in Cape Town NHI was discussed by Prof Di McIntyre of the health economics unit of the University of Cape Town’s School of Public Health and Family Medicine, and by Dr Jonathan Broomberg, general manager of strategy and risk management at Discovery Health.
Although there’s no formal NHI proposal on the table yet, Broomberg warned that implementation of the plan may be ideologically driven rather than by what is practical.
McIntyre said that while there’s no doubt NHI will be implemented, “the final form is not certain nor set in stone. The challenge is to identify each group’s role. Those in the private sector must work out how they will fit into the system and how NHI will remunerate them for their role”.
We provide an in-depth look at NHI: Is there a place for NHI? What are the practical pitfalls? How could it work? And how will the plan affect the medical community?.
The case for NHI
View from the academic sector
South Africans with the greatest need for healthcare have the least access to it – obviously health financials must change
Most of the statistics below come from the Shield study (Strategies for Health Insurance for Equity in Less Developed countries) undertaken by McIntyre and colleagues in South Africa, Ghana and Tanzania. The study is funded by the European Union.
South Africans are ready for NHI – they’ve had enough of the health system as it is, says McIntyre. “In a survey, three quarters of medical scheme members indicated they would join NHI if it were cheaper than their current medical scheme.”
The present system is untenable
When it comes to income inequality,
South Africa is right up there in the
number one spot in the world, with the
richest 10% of our population earning
more than half the income in the country.
Access to medical resources is just as unbalanced with, for example, a general doctor-to-patient ratio of about 1:4 000 in the public sector and 1:558 in the private sector.
Moreover, spending by medical schemes per beneficiary almost doubled between 1996 and 2006, while in the public sector spending per person decreased a bit in this period before returning to what it was ten years prior, McIntyre says.
In the past ten years, the public health system has become systematically under-resourced: while the number of staff has declined, healthcare needs have increased as a result of HIV/Aids, XDRTB and the growing burden of noncommunicable diseases. Staff morale is low and there’s a perception that the quality of healthcare in the public system is declining.
“With such huge inequalities, it’s obvious that health financials in the country have to change,” McIntyre says.
Available resources don’t benefit those who need them
The poorest people in South Africa have
access to only 13% of all the available
benefits, while the richest get 36% of the
benefits, McIntyre says.
"That would be fine if the rich were sicker or in greater need of healthcare, but the opposite is true. The Shield study showed that the poorest of the population experience 25% of the need for healthcare available in South Africa, as opposed to the richest segment which only has 9% of the healthcare need."
The resources drawn into the South African health system therefore don’t benefit those who need it most.
Current funding is flawed
1. Tax inequalities
South Africa has quite a progressive personal income tax system, in which the rich pay a far greater portion of their income towards personal tax than poorer people.
But our other taxes are not quite as progressive. The Shield study showed that South Africa’s poor bear a greater burden of excise tax, fuel levy and even corporate tax than the rich (that’s because corporate tax is eventually reflected back to consumers).
"As a result, quite a significant portion of the income of poorer households ends up in the taxman’s pocket," McIntyre explains.
2. Medical aid scheme inequalities
Healthcare is directly funded in three ways: out of patients’ pockets, by medical aids, and by the 11% of general tax revenue that’s allocated to healthcare.
The Shield study showed that of these three, the only instance where rich people contribute significantly more than poor people, is in the case of medical aid schemes – from which the poor don’t benefit anyway. Only 14% of South Africans belong to medical aid schemes.
NHI in a nutshell
Government has committed itself to restoring public hospitals so they can once again be the backbone of the system.
The quality of these hospitals should
eventually be such that they will be the
provider of choice for the vast majority
of South Africans.
“Some ways of achieving this would be to improve conditions for healthcare staff and give management more autonomy while also making them more accountable,” McIntyre says.
Private doctors will be encouraged to participate in the NHI scheme.
Income inequalities
Share of income for richest 10%
Increased from 47% (1995) to 51% (2005)
Share of income for poorest 10%
Decreased from 0,5% (1995) to 0,2% (2005)
The concerns about NHI
View from the private sector
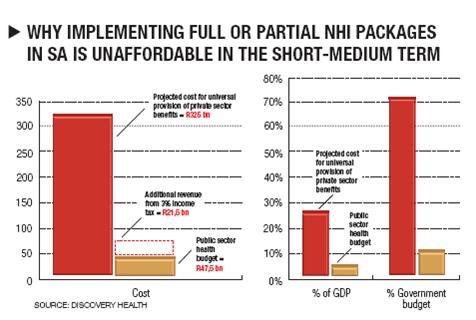
Our economy cannot currently afford to offer the package of health services available in the private sector, to the whole country
NHI could be an excellent solution to South Africa’s healthcare inequality problems, but not in the short or medium term, and certainly not within the five years envisaged by the ANC’s election manifesto, say experts.
It should be implemented gradually, with mandatory cover slowly but surely being extended as the extent of formal employment and the tax base expands, and as various infrastructures – such as quality public hospitals, sufficient human resources and efficient administration systems – come into effect.
As the plan currently stands, it is not realistic, Broomberg says. “Our economy cannot afford to provide the comprehensive package of health services that can currently be bought through medical aids, to everyone in the country. This means NHI will only be able to provide a limited range of services to the entire population.”
Why the NHI plan is unrealistic
Too little money
Millions of South Africans are unemployed and therefore unable to contribute to NHI. Of the small number who are employed and pay tax, many will find it difficult to afford another 3-5% to pay into an NHI system.
And even if they can afford it, it still won’t be nearly enough to fund the total healthcare package currently purchased by the average medical scheme member.
“Discovery estimates that to extend such a package to the entire population would cost about R325 billion, leaving a shortfall of more than R250 billion,” Broomberg says.
This will lead to very limited coverage, and as a result there will still be significant demand for access to the high-quality private healthcare services the eight million members of medical schemes currently have access to.
The ANC NHI committee seems to believe that eliminating medical schemes will automatically bring private funding and private providers into the NHI system, and that the R64,7 billion currently flowing through medical schemes will go to NHI.
“However, this won’t happen,” Broomberg warns. “Consumers who are able to afford private care will continue to purchase this, but they will do so in the absence of the cross-subsidies and risk pooling the current medical schemes provide.
Moreover, if private hospitals can’t get enough income through the NHI system, they may either shut down or find other ways to raise income. Similarly, doctors will remain in private practice or exit the system or the country if they’re not able to earn what they believe they should be earning.”
Too few resources
Before an NHI package similar to what
can currently be bought through medical
schemes can be extended to the whole
country, the following is needed:
60 000 more hospital beds
320 000 more nurses
124 000 more doctors and specialists
Too little admin capacity
If district health authorities can’t cope
with the current service delivery, how
will they contract and manage public as
well as private providers?
Healthcare procurement is highly complex, and large public health authorities throughout the world struggle with this, Broomberg says. How will district units be able to achieve it within five years?
If medical schemes should disappear
The money flow in medical schemes
will not simply go to NHI, and doctors
and nurses in the private system will not
automatically move into the public system,
Broomberg says.
People will still use their private money to purchase private healthcare, and just pay cash for it.
Private doctors will either work for cash or leave the system. Private hospitals will also work on a cash basis. There will be a skills flight, which will undermine government’s retention strategy.
Foreign investment will be discouraged, and there’s a risk of significant damage to and loss of skills and infrastructure.
Making NHI work
Starting small
Accept that initially NHI will only be able to
provide a small and very partial package.
It won’t meet the demand of those able to afford a more extensive package, and it won’t be able to fund the services of the majority of doctors and private hospitals, says Broomberg.
Improving the public healthcare system
A substantial increase in funding is
needed for this. As the system
improves, NHI can be expanded.
Expanding a regulated medical scheme environment
“Government could start by implementing the Risk Equalisation Fund (REF),” Broomberg suggests. This is a fund to
which medical aid schemes with healthier,
younger members contribute to help
subsidise those schemes with sicker
members.
“Cross-subsidies from the Treasury into the REF will make it easier for people with a low income to join. More low-income medical schemes (LIMS) should be established, and finally, mandatory cover can be initiated progressively as the economy allows,” Broomberg says.
Working with the private sector
Better coordination and collaboration
between the public and private sector is
critical. “Private healthcare is a national
asset. Last year it was ranked sixth in
the world in terms of performance on
access and quality. It should be used as a
platform for the NHI system,” Broomberg
says.
And, ultimately
Once all the building blocks above are
in place, public and private financing
pools can be integrated into one NHI –
providing there is universal access to a
comprehensive package.
NHI funds can purchase defined services from both public and private providers, while private health insurance should be maintained to provide duplicative, complementary or top-up services to those willing to contribute.
How the ANC sees NHI
This is how the ANC envisages NHI in its election manifesto
NHI will be publicly funded.
Contributions will be made according to
the ability to pay.
- Administration
The NHI system will be publicly administered. - Implementation
Public sector standards must first be raised.
Private doctors will be encouraged to participate in the NHI scheme, provided they are in group practices and willing to accept capitation fees at levels determined by the NHI authority. - For patients
Access will not be determined by contributions; services will be free at the point of delivery.
There will be a choice of service providers within a district. - Principles
Primary healthcare, hospital services and outpatient services will be free at the point of service.
There will be private and public facilities and providers.
An independent quality improvement and accreditation body will set the national standards.
Envisaged over five years.
Funding: The current 11% allocation of general tax revenue to health services will be increased to 15%. Taxpayers will probably pay an extra 3-5% personal income tax to help fund NHI.
All relevant healthcare services are to be funded by the NHI through a centrally administered NHI fund.
This central fund will channel funds to district health authorities (DHAs).
The DHAs will contract with public hospitals and clinics, and also with private group practices on a capitation basis.
The role of medical schemes will be reduced to providing top-up cover for services not funded by NHI, such as cosmetic procedures. They will be prevented from covering services that are already covered by NHI.
Sources: Discovery Health, Financial Mail
How NHI will affect doctors
The exact position of doctors – especially private doctors – within an NHI system is not yet clear. There have been suggestions that private healthcare and medical aid companies should be completely eliminated, but according to McIntyre, this is unlikely and based on minority views.
Observers say the lofty idea is that eventually the quality and working environment of the public healthcare system will be such that general doctors and specialists will want to work there, and the best medical minds will vie for professorships at tertiary institutions, which will be centres of excellence.
As a result, the public healthcare system will be the provider of choice for patients. Private GPs will be encouraged to participate in the NHI scheme by forming high-quality primary healthcare practices manned by them, primary healthcare nurses and allied health professionals such as physiotherapists.
These accredited NHI providers will serve as gatekeepers in the health system and patients will be encouraged to go to them rather than straight to hospital. They will be remunerated by government on a capitation basis rather than a fee-for-service basis. The level of remuneration will be set by the NHI authority.
Citizens would be able to choose between accredited providers in their area. It’s not clear if and how private healthcare as we know it will exist outside the NHI model. There will definitely be a place for private top-up services that are not covered by NHI, such as cosmetic surgery, and possibly a smaller version of what we currently have for those patients who insist on using private healthcare.
However, it seems unlikely that the current private health system will disappear any time soon, as NHI will initially not be able to provide services of the same quality and with the same accessibility as can currently be bought through medical aid schemes.
This is an edited extract of an article first published in What’s New Doc, 3rd issue, March/April 2009. What’s New Doc is a publication for medical doctors, produced in association with Health24.
Read more:
For some startling facts and figures, click here.




 Publications
Publications
 Partners
Partners