A chronic illness is so much more than discomfort and constantly checking into the hospital. “Socially it’s been the biggest problem,” Maddie Beale, a Crohn’s disease sufferer, says. Just over a week ago today marks a year since she was diagnosed with Crohn’s.
“You end up in the hospital and people are all gaga to come visit you for the first admission, or the second one… and then eventually it’s, ‘Ag she’s back there again! That’s so annoying.'”
Chronic illnesses are often invisible. There is constant pain that, as a friend of a sufferer, can be hard to relate to. Here is the truth about this disease, as told by Maddie.
Crohn’s disease: the diagnosis
“It took a while for me to be diagnosed, but it actually wasn’t as long as [it takes for] a lot of people,” Maddie begins. “Looking back, I realise that I’ve had symptoms for years!”
But the journey towards a diagnosis really began in October 2016. “Something just wasn’t right. My heart was racing and I was so tired; I had an upset stomach that just wasn’t going away,” Maddie says. Her GP wasn’t convinced, but sent her for blood tests. “I went straight from Pathcare to the hospital,” she says.
After a week of hospital tests, Maddie was told her intestines were inflamed. “But the doctors decided to treat it as if it’s acute and sent me home, loaded with antibiotics and steroids,” she said. It didn’t get better, and around February last year, she found herself back in the hospital.
After a CAT scan and urine samples, she was sent home yet again, having been told she was fine and was simply trying to get a day off varsity. “I couldn’t move. I was in screaming pain,” she recalls.
Read more: The truth about chronic inflammation and what it means for your health
In March, Maddie and her family decided to take things into their own hands. They made an appointment with a gastroenterologist (a doctor who specialises in conditions of the digestive tract).
“I explained my whole story and he said he could probably confidently diagnose me from just this.” After an MRE scan, which provides the doctor with detailed images of the small intestine and bowel, the expert confirmed his suspicions: Crohn’s. “It was a long process, but I know some people that took four or five years to diagnose. It could have been a lot worse…”
Dealing with Crohn’s
Finding out that you have a chronic illness is far from fun. “[But] in a way, you feel so relieved,” says Maddie. “After being told that you’re just making it up and it’s all in your head… There is a reason – that’s a relief.” But, of course, it’s also devastating. “You tell yourself that you’re fine, that you’ll get a course of antibiotics and then everything will be okay. You want people to understand that the pain is real, but you don’t want to be stuck with it forever.”
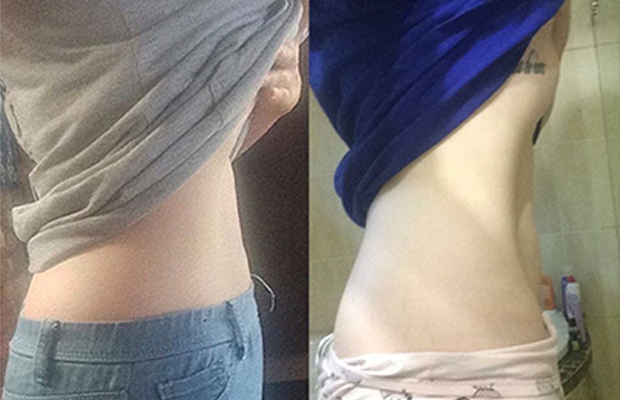
“My symptoms are much better now, but in the beginning – uncontrolled diarrhoea,” Maddie says with a laugh, “That’s why no one wants to talk about Crohn’s – because it’s ugly.” The symptoms include major blood loss through the ulcerations on your intestines. “I experienced massive weight loss. I dropped 10 kilos – like that!”
It was scary, yet Maddie still had people telling her how lucky she was to lose weight so quickly. “No, that’s not fun. What’s fun is going and working out – just having your weight fall off you is not nice.”
Read more: “I developed an invisible illness – here’s what it’s like”
Fatigue is another symptom. “That is probably my main struggle now,” Maddie adds. There are other things that she didn’t even think would be connected to this disease. “I had ulcers in my mouth all the time and my eye sight [was affected].”
Then there’s the pain, which includes severe joint pain because Crohn’s causes inflammation everywhere. Not to mention the lack of appetite and subsequent weight loss. “I had seven hospitalisations last year because my symptoms were just too much to handle.”
The treatment
Maddie was first put on a high dose of cortisone. “Anyone who has ever been on cortisone can tell you that it’s the worst thing ever,” she adds. “It makes you swell up and get a nice round moon face.” A side effect of cortisone is insomnia. “You’re so exhausted and feeling so sick, but you’re also buzzing.”
Maddie then went on to Imuran, a drug used to stop organ rejection after organ transplants. “It’s an auto-immune disease so the best thing is immunosuppressants – if you just wipe out the immune system…” she explains. But this made her so ill that she ended up with pancreatitis.
“I’m now on Mezavant. It’s much milder, but I’m on a high dose and it seems to be controlling things. It doesn’t damage your immune system and I’m really hoping that I can stay on it for as long as possible!”
Living with it
“Obviously my diet has changed a lot – I go through stages when I’m just on baby food,” Maddie says. There are a lot of foods she’s had to give up too: “I’m not allowed to eat anything high in fibre – the more processed, the better it is for me.” Any vegetables need to be cooked to mush. “When I explain what I can eat to people, they get a bit of a horrified look on their faces. I can eat that McDonald’s, but no salad for me!” Her favourite snack, nuts – out. “And no popcorn! How do I go to the movies now?” She jokes.
Varsity life has been a bit of a tricky adjustment. After the 45-minute drive to campus, “I’ve got a full day sitting there and I’m in pain. I don’t want to eat, but then I get low blood sugar so I’m shaky and miserable. I end up just staying home. My lecturers have been really supportive, though. I did fail a couple of subjects last year, but I’m impressed I passed what I did because I missed so much!” This year is going much better with the new meds.
Read more: What this Instagram yogi wants you to know about living with chronic pain
“Socially it’s been the biggest problem,” Maddie says. At first, friends are understanding when you say, “I can’t come out with you because I’m not doing well, or I’m too tired, or I can’t drink because I’m on medication and it will kill me if I do.” But the sympathy turns to irritation quite quickly, especially when there’s nothing you can physically see. “But you also learn who your real friends are really quickly,” she adds.
Another thing that was especially rough was the lack of independence. “I went through a stage when I couldn’t even get out the bath on my own,” Maddie says. And when it came to Christmas shopping, she did it by wheelchair. “You realise the prejudices people have – they assume that if you’re in a wheelchair, your legs don’t work. Anything else and you’re just being lazy.”

Maddie’s advice to fellow Crohnies
“The main thing, and I think this goes for anyone who has any form of chronic illness, is not to let it define you. It is a big part of your life, but don’t make your life about the illness.” It’s an easy pit to fall into and Maddie says she’s been there. “You can be so sick and just go into a ball of pity,” she adds. “But you are perfectly capable of carrying on with your life.”
Maddie has made many friends with Crohn’s or other chronic illnesses through Instagram. It’s so important to have a support system, “and just because they’re a stranger you met online doesn’t mean they won’t understand you – maybe they will [understand you] even better than those directly in your life.”
And finally, “don’t throw away your goals and dreams – adapt them! No one is ever going to look down on you for changing the way you reach your goals. Just do it.”
This article was originally published on www.womenshealthsa.co.za
Image credit: Supplied




 Publications
Publications
 Partners
Partners














