Men are generally keen on breasts, unless they start growing their own. Breast enlargement in men, known as gynaecomastia, is a common occurrence amongst males of all ages.
According to Cape Town plastic surgeon, Stuart Geldenhuys, the reduction of male breast enlargement, known as gynaecomastia surgery, is ranked as one of the top five cosmetic procedures performed on men. Gynaecomastia surgery, otherwise known as reduction mammoplasty, is the removal of excess glandular tissue or excessive fatty tissue in the male breast. In more severe cases removal of lax skin is also required.
What is gynaecomastia?
Gynaecomastia is the abnormal enlargement of one or both breasts in males due to the benign proliferation of breast glandular tissue. In some cases lactation / milk production may be present.
Pseudo-gynaecomastia is a different condition distinguishable from gynaecomastia in that it occurs in obese men and refers to enlarged breasts due to fat deposition, without glandular proliferation.
Gynaecomastia on occasion must be differentiated from breast cancer, which is far less common and is typically unilateral.
Case study success
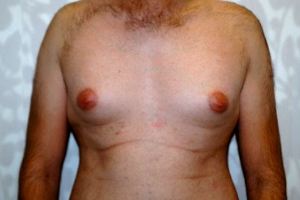
One of Dr Geldenhuys' patients, Mr X had the surgery done and said before he had it done he tried to cover up and hide it and would avoid wearing t-shirts as he felt his breasts were too prominent.
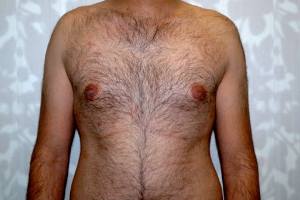
Before and after images of Mr X.
"It was a difficult decision to have the surgery. I had always wanted to have something done, but I did not know about the procedure. The turning point was speaking to a friend who worked for a medical aid and said it was quite common, and that it was not risky. I felt it would make a difference in my life, understanding that it was not only a physical issue, but an emotional issue as well."
Following the procedure he said, "There has been a significant reduction in the size of the breast tissue on my chest, especially from a side view, but if I look down, I still see breast tissue. It has been two and a half months since the operation, and Dr Geldenhuys said that the final result will only be visible after a year. I am, none the less happy with the immediate effects. The operation was basically painless: I was put under and remember waking up still asking if they started yet. I had to remain in bed for about two weeks, but the pain was not unbearable.
"I now feel confident to wear t-shirts, and suit jackets. I don’t look at my chest in the mirror when I get dressed to see if my breasts are bulging through. I went on a holiday recently and for the first time I was confident enough to walk on the beach- topless.
How do I know if I have gynaecomastia?
Gynaecomastia, a male condition, is any growth of the glandular tissue in a male breast. Carefully feeling the area beneath the nipple areola region, often by pinching the deeper tissue, will reveal a discreet area of thickening.
In some publications it is arbitrarily defined as a palpable sub-areola gland or mass greater than 2cm. In severe cases this area of thickening is larger and the chest looks more typical of a typical female breast.
Men sporting a pair of enlarged breasts, inevitably feel uncomfortable taking their shirts off in front of others, and may avoid certain physical activities and even intimacy, in order to hide their condition. Simple, every day clothing choices are influenced by having gynaecomastia, avoiding circumstances where the excessive breast protuberance is more evident.
Dr Geldenhuys says that in his experience, gynaecomastia is a source of embarrassment, intense frustration and mental anguish necessitating modifications to many aspects of a patients daily routine and lifestyle.
Thankfully gynaecomastia surgery offers sufferers the opportunity to regain their confidence. Despite this, many men are too self conscious to seek assistance.
What causes breast enlargement in men?
According to Dr Geldenhuys there are a variety of reasons for the over-development of male breast tissue.
Gynaecomastia is a complex condition resulting from alterations in hormone levels, which act on breast tissue. Estrogens strongly stimulate breast tissue development, while androgens inhibit breast growth.
Several hypotheses exist to explain the etiology of gynaecomastia including; increased levels of oestrogen, too little free testosterone or the sensitivity of breast tissue to circulating hormones.
Physiological or idiopathic gynaecomastia, which accounts for by far the most cases of gynaecomastia occurs typically in three distinct periods.
It is estimated that in the perinatal period 60-90% of males at birth have some degree of breast development due to trans-placental passage of oestrogens.
At puberty 50-60% of boys aged between 10 and 16 years may have some breast tissue growth but the true incidence, although not known, is thought to be less than 5%. Pubertal gynaecomastia resolves spontaneously in most cases.
Finally ‘involutional’ gynaecomastia typically occurs after the age of 50 in up to 80% of men due to falling androgen levels.
Medications implicated include; Anti-anxiety medications, antidepressants, Antibiotics, Ulcer medications, anabolic steroids, androgens, growth hormones, the use of estrogen creams, chemotherapy, certain heart medications and drugs prescribed for HIV, drug and alcohol abuse. Street drugs such as marijuana, amphetamines and heroin, and alcohol abuse are known to be causal.
Conditions that interfere or change normal testosterone production such as hypogonadism, hyperthyroidism, are also commonly associated with enlarged breasts in men.
Geldenhuys adds that kidney and liver failure, cirrhosis, injuries to the chest wall or spinal cord, genetic disorders and certain tumours have also been shown to be the underlying causes of enlarged breasts. Hormone-secreting tumour of the lung, or other organs may rarely be implicated.
The most important differentiation is between gynaecomastia and breast carcinoma. Male breast cancer is rare but should not be missed. It is generally unilateral, does not necessarily occur behind the nipple, is hard or firm, and may be associated with skin dimpling, nipple retraction or discharge.
Less common local causes of unilateral breast enlargement include neurofibromas, lymphangiomas, hematomas, lipomas, and cysts.
Patient evaluation
Most cases of gynaecomastia have no associated pathology and are not associated with any other disorders - typically referred to as ‘idiopathic’ - it is a diagnosis by exclusion of rarer causes.
The first step in the clinical evaluation of gynaecomastia, is the elimination of pseudogynecomastia and carcinoma as causes of enlarged breasts. A formal examination and if necessary imaging tests to identify the cause of the disease.
Laboratory tests for assessing liver function tests, kidney and thyroid function, blood testosterone, Luteinizing hormone (LH), Human chorionic gonadotropin (HCG) and estrogen levels respectively may also be required.
Puberty occurring gynaecomastia disappears spontaneously for most teenagers in less than three years, but patients should be kept under observation. Unfortunately, puberty occurring gynaecomastia has a negative impact on the personal image of adolescents and may lead to depression.
In adults with asymptomatic gynaecomastia, no treatment is required. Men who experience pain or soreness need short-term treatment. If it turns out that gynaecomastia is caused by the use of any drug, improvement in the situation can be seen in more than a month after the patient stops the use of that certain drug.
For chronic gynaecomastia, it is unlikely for the disease to regress spontaneously. In these cases, subcutaneous mastectomy or liposuction can be considered. Liposuction alone may be sufficient in cases where breast enlargement is caused by excess fatty tissue - pseudogynecomastia.
How is gynaecomastia surgery performed?
Gynaecomastia is usually treated by a combination of liposuction and surgical excision. In cases of pseudogynaecomastia (excess fatty tissue), liposuction techniques alone may be used.
These procedure are usually performed under general anaesthesia or deep intravenous sedation and patients are generally not required to stay in hospital overnight.
“Liposuction involves inserting a cannula (a thin hollow tube) through a small 2-3mm incision. The cannula, attached to a vacuum device, is moved back and forth, in a controlled motion to both mobilise and remove the excess fat. The liposuction also serves to contour the chest shape, further enhancing the overall result.
Excision techniques are employed in most cases of gynaecomastia. The specific technique used varies depending on the size of the breast or glandular tissue present and the amount of skin excess requiring excision. Incisions are confined to the areola border, where possible, so as to limit visible scarring.
The results
The expected final results of gynaecomastia surgery results in flattened natural male breast shape and enhanced chest contours specifically removing the appearance and stigmatisation associated with the female breast. In most cases the scars can be concealed in the areola margin or natural contours of the breast.
Whilst not typically a particularly painful procedure (return to ‘sedentary’ work after a week is usual) swelling does persist for many months and skin contraction and remodelling are required to attain the final result.
Dr Geldenhuys cautions that if breast enlargement was caused by the use of certain prescription medications, drugs including steroids or weight gain, the patient must be fully free from these substances and remain at a stable weight in order to maintain the results.
Risks associated with the procedure
Like any surgical procedure gynaecomastia Surgery carries its own risks. Dr Geldenhuys emphasises that complications are relatively uncommon, especially when the procedure is performed by an experienced surgeon.
“As with all procedures, bruising and swelling are to be expected from gynaecomastia surgery, but it usually dissipates within two to three weeks following the procedure. Some patients also report itchiness and dry skin, especially around the incision sites. Post operatively scar management regimes including taping, topical creams and silicone are employed.
“It is not at all uncommon to experience discomfort and altered sensations in the breasts following the procedure. However, this is temporary and usually goes away after the operation,” says Geldenhuys.
The most common complications include haematoma (collection of blood) which may necessitate a return to theatre for drainage.
Gynaecomastia is typically asymmetric and as each side of the chest needs to be worked on separately; contour and shape irregularities may occur after gynaecomastia. If this occurs, revision surgery may be required after six months.
All surgery leaves scars, some more visible than others. Although good wound healing after a surgical procedure is expected, abnormal scars may occur within the skin and deeper tissues. The amount of scarring usually depends on the extent of tissue to be removed. Scars may be unattractive and of different colour than the surrounding skin . In the event that scarring is too prominent, many treatments are available to reduce their visibility.
The occurrence of enlarged breasts in men is increasing and it remains a fact that the psychological damage done as men battle with their self-image and withdraw from many aspects of their lives is not to be underestimated. Gynaecomastia surgery is a safe and effective solution to an embarrassing problem for many men.
Reference: Dr Stuart Geldenhuys
(Health24, July 2012)
Read more:
Breast reduction: before and after




 Publications
Publications
 Partners
Partners