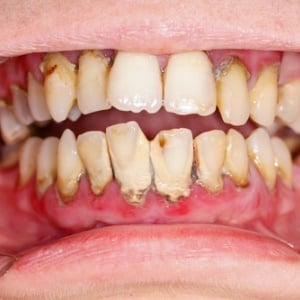
Do you suffer from:
- Gums that bleed easily, such as during brushing or flossing?
- Red, swollen or tender gums?
- Gums that have pulled away from the teeth?
- Persistent bad breath?
- Loose or separating teeth?
- A change in the way your teeth fit together when you bite?
- Are you over 30?
Periodontal disease is responsible for more than 80% of tooth loss after the age of 35. It is second only to the common cold as the most common of human diseases and is found in more than one in three people over the age of 30.
There is a definite connection between periodontal infection and more serious health problems, such as cardiovascular disease, diabetes, respiratory disease and pre-term birth weight babies.
What is periodontal disease?
Periodontal disease is a slow, progressing, chronic infection that affects the structures supporting the teeth, and is caused by bacteria found in plaque. These supporting structures are the gums and the bone that hold the teeth within the jaws by means of fibres known as the periodontal membrane.
This infection can affect only one tooth at a time, or multiple teeth simultaneously, and starts as the sticky white layer of plaque that constantly forms on your teeth.
How does periodontal disease appear in the mouth?
There are two main types of periodontal disease, gingivitis and the more destructive periodontitis.
Gingivitis
Gingivitis presents as gums that bleed when brushed or sometimes even when just touched. The gums gradually become red, swollen and move away from the teeth forming pockets. There may sometimes be an acute phase (known as "trench mouth"), when there may be some pain. Generally, the condition is painless and causes so little discomfort that it is often neglected for many years, until diagnosed by a dentist.
Gingivitis is caused by inadequate oral hygiene, which results in plaque build-up. It can be reversed with professional treatment and good oral home care.
Periodontitis
When gingivitis is neglected, the inflammation may extend deeper into the tissue. Toxins produced by the bacteria in the plaque irritate the gums. The toxins stimulate an inflammatory response in which the body in essence turns on itself, and the tissues and bone that support the teeth are broken down and destroyed. The gums separate from the teeth, resulting in the formation of pockets (unnatural spaces between the teeth and the gums). These act as breeding grounds for bacteria and will eventually fill with puss.
More bone and gum tissue is destroyed as the disease progresses. The inflammation thus extends into the bone surrounding the teeth, which may then become loose, drift out of position and will eventually be lost. Gum abscesses may form at any time during the above course of events.
An advanced state of periodontal disease can be reached without having experienced any pain or discomfort.
Plaque
Bacteria are normally present in the mouth. In order to cause periodontal disease, they must remain undisturbed at the margin where the gum meets the tooth, particularly in between the teeth. They accumulate and multiply in the form of an invisible film known as plaque.
Plaque starts to accumulate on the tooth at the gum margin almost immediately following its removal. However, it takes 12-24 hours for the plaque to become harmful to the gum tissues. Wherever plaque is not removed, it may cause periodontal disease.
Plaque, together with some constituents of the saliva, form tartar (calculus). This is a hard crust-like material which is deposited on the teeth and on which a further deposition of plaque takes place, thus increasing the amount of calculus. Once formed, calculus cannot be removed by tooth brushing and should be removed by a dentist or dental hygienist with special dental instruments.
Other common sites for the formation of bacterial plaque are:
- worn out fillings;
- poor fillings or crowns with overhanging edges;
- badly decayed teeth;
- wedging of food particles between teeth into the gums during chewing;
- partial dentures, particularly plastic dentures.
Other risk factors that can affect the severity and speed of development of periodontitis include:
- the use of tobacco products;
- stress;
- genetics;
- hormonal changes such as during pregnancy, menopause or post-menopause;
- poor nutrition;
- people older than 55, since more than half of people aged 55 and older have periodontitis;
- HIV/Aids sufferers;
- Xerostomia (dry mouth syndrome);
- osteoporosis and arthritis which may make brushing and flossing difficult.
Why should periodontal disease be treated?
The main reason for treating periodontal disease is to preserve the natural teeth and bone. Without treatment, destruction of the surrounding tissues of the teeth will occur. Extensive dental treatment, including crown and bridgework should only be done in a mouth free of periodontal disease.
How can periodontal disease be prevented?
Correct oral hygiene will prevent the formation of bacterial plaque and keep the gums healthy. Learn the correct teeth cleansing technique. Visit the oral hygienist regularly to have calculus removed. Have regular periodontal examinations and periodic x-rays to reveal otherwise undetectable changes in jaw bone. Remember there will usually be no pain or discomfort to warn you.
Do antibiotics play an important role in the treatment of periodontal disease?
Yes. Antibiotics, particularly tetracycline, are essential as adjuncts to the treatment of certain aggressive forms of the disease. Antibiotics are often administered to prevent post-treatment infection when surgery has been extensive. Although periodontal disease is of bacterial origin, antibiotics alone are not a solution to the eradication of the disease.
How long will the treatment take and how much will it cost?
This will depend on the nature and severity of the disease. Generally, the fee has a direct proportion to the treatment time involved as well as to the complexity of the procedures required. Besides repairing the damage that has resulted, your dentist and dental hygienist may have to spend several hours teaching you correct oral hygiene procedures and checking your progress at frequent intervals. Certain cases may be referred to a periodontist (a dentist that has specialised in treating periodontitis).
What does treatment entail?
In order to assess the state of health in your mouth, a dentist must examine your mouth and, if your suspicions are confirmed, a detailed clinical examination must be undertaken. This examination consists of inspection of the gum, measurements of the extent of gum destruction around the entire mouth and the taking of a set of full-mouth radiographs.
Treatment usually consists of the following:
- Learning an effective oral hygiene technique.
- Having your teeth scaled and polished.
- Root planing - where an attempt is made to decontaminate the surfaces of the roots of your teeth using special dental instruments in order that the gum may become re-attached to the tooth surface. This usually requires local anaesthetic.
- Where the periodontal condition is advanced, minor surgical procedures may be necessary to gain access to the roots requiring decontamination, as well as to correct any major changes that may have resulted from the disease.
Each patient will have different problems which will have to be handled on an individual basis. Discuss these with your dentist.
Will treatment ever have to be repeated?
Usually not. Sometimes an isolated area may require further treatment. With regular periodontal maintenance therapy, treatment may never have to be repeated. During maintenance therapy, screening will be carried out to ensure that your oral hygiene technique remains efficient and to detect and treat any recurrence as early and as simply as possible.
Should periodontal disease recur due to poor oral hygiene or failure to attend for maintenance, repeating periodontal treatment would be futile.
What happens when treatment has been completed?
You will be scheduled to commence a periodontal maintenance programme which will usually consist of three-monthly visits to the oral hygienist. This interval may be reduced or extended depending on several factors such as the original severity of the disease and your ability to effectively remove plaque.
Can periodontal treatment be guaranteed?
No. It is against the law for members of the dental or medical profession to guarantee treatment. We are dealing with a biological science in which response to treatment usually varies. We can, however, guarantee that, once treated, the disease will recur in the presence of plaque.
Can periodontal disease be inherited?
No. Many experts, however, feel that it is possible to inherit a predisposition to periodontal disease, particularly the advanced forms of the disease.
Is periodontal disease contagious?
The bacteria that cause periodontal disease can be passed through saliva. This means the common contact of saliva in families puts children and couples at risk of contracting the disease of another family member.
Why do some people who look after their mouths fairly well suffer from periodontal disease whereas others who hardly ever use a toothbrush do not?
We still do not know the answer to this. Recent research has given us some clues. We must accept the fact that some individuals are more susceptible to periodontal disease than others. In the absence of plaque, periodontal disease will usually not occur irrespectively of whether one is susceptible to the disease or not. Patients who require periodontal treatment must be regarded as being susceptible to the disease for the rest of their lives. In the absence of efficient oral hygiene recurrence will occur.
- (Dr Ilona Visser/Health24)




 Publications
Publications
 Partners
Partners














