Angioplasty - also called PTCA - is a common medical procedure, performed in a special cardiac catheterisation theatre. Not all patients or types of blockages are suitable for angioplasty. Some of the more common procedures are:
Types of angioplasty
Balloon angioplasty
In this procedure, a fine tube, or catheter, is threaded through an artery into the narrowed heart vessel. The catheter has a tiny balloon at its tip. The balloon is repeatedly inflated and deflated to open and stretch the artery, improving blood flow. The balloon is then deflated and the catheter is removed.
Rotational atherectomy
This process is a mini version of a router used to unblock drains. A rotating diamond-headed burr drills its way through plaque, opening up the artery to let blood flow again.
Directional atherectomy
Here, a special catheter with side-blades is used, which cuts long slits down the length of the plaque. This allows it to "expand" in place, letting blood flow freely.
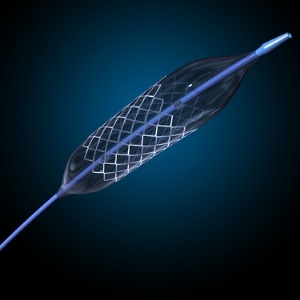
PTCA plus stent
Doctors often insert a stent after the angioplasty procedure. An expandable wire mesh tube, the stent, is positioned in the artery where the blockage was, and this is used to keep the artery open after an angioplasty. The stent stays permanently in the artery.
Once a stent has been used, the patient must be on anti-platelet agents (specific anti-clotting drugs) for a minimum of 6 months, and sometimes for a year or more. Because the stent is foreign to the body, clotting is stimulated. A clot inside the stent would totally block it off, so this must be prevented from happening.
Stents may be made of bare metal, or of metal coated with different drugs to suppress the inflammatory response and delay further atheroma formation. Unfortunately many of these drug-eluting stents (DES) aggravate the problem, and re-narrowing can occur either within the stent, or at either end of it. This may happen to up to 30% of patients within six months of the original DES being inserted.
This is also more likely to happen if the patient smokes, or has diabetes or unstable angina. Stented vessels that re-close may be re-opened with another angioplasty, or may be referred for coronary artery bypass grafting.
Risks
Angioplasty is an invasive procedure, carrying risks common to any surgery such as bleeding and infection. There are added risks in particular, because these patients all have coronary artery disease, and the guide-wires and catheters can damage or perforate the heart muscle or valves. As the catheter is inserted into the coronary artery, a flap of tissue or atheroma can be lifted up - this is called a dissection, and can be life-threatening, needing IMMEDIATE bypass surgery. A common problem is post-operative bleeding from the site in the groin where the catheter is inserted: bleeding may be severe enough to require a blood transfusion.
During the angioplasty, small bits of plaque can break off and be carried further down in the artery, blocking it off, and thereby causing a heart attack.




 Publications
Publications
 Partners
Partners











