Summary
- Tonsillitis is an infection of the tonsils, the small masses of lymphatic tissue at the back of the throat.
- Tonsillitis most commonly affects children between the ages of one and seven.
- Tonsillitis is usually not serious, unless a tonsillar abscess – a collection of pus behind the tonsils – develops.
- Obstruction to breathing by enlarged tonsils may cause snoring and disturbed sleep patterns.
- Bacterial infections can be treated with appropriate antibiotics. Viral infections do not respond to antibiotics.
- Tonsillectomy is performed in cases of recurring or serious infection, or for significant airway obstruction.
Description
Healthy tonsils
- The tonsils are the two small masses of lymphatic tissue lying on either side of the uvula, (the "little-tongue" of the soft palate). With the adenoids, they form part of a ring of glandular tissue at the back of the throat.
- Healthy tonsils are small, pinkish lumps of tissue, much the same colour as the surrounding area. Usually the two tonsils are of about equal size.
- The popular belief that the tonsils "filter out" bacteria is a myth; but doctors do think that the tonsils may assist in defending the body against bacteria and viruses by helping to form antibodies. However, this help may only be significant during the first year of life, if at all – there is no evidence that the tonsils play an important role in immunity. Studies show that children who have had their tonsils and adenoids removed do not suffer from compromised immunity.
Tonsillitis
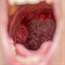
- When viruses or bacteria infect the tonsils, they become red and swollen, and can develop white or yellow spots. This condition is called tonsillitis. A persistent or recurring infection of the tonsils is called chronic tonsillitis.
- Tonsillitis is most common in early childhood. This is probably when the tonsils are most involved in fighting disease. As one gets older, the tonsils become smaller and are less prone to infection.
- Tonsillitis is generally not a serious problem. However, if a tonsillar abscess develops, the swelling can be severe enough to obstruct breathing.
- Secondary ear infections from the associated adenoid problems can also occur with acute tonsillitis.
Peritonsillar abscess
A peritonsillar abscess develops when pus collects behind the tonsils. This can push a tonsil toward the uvula. This condition can be extremely painful, and may make it difficult for the patient to open his or her mouth. If it is not treated, the infection can spread down deeper into the neck, obstructing the airway. Complications from this abscess may be life threatening.
Enlarged (hypertrophic) tonsils
Infection and even chronic allergy can cause the tonsils and adenoids to become greatly enlarged. This may obstruct breathing, causing snoring and disturbed sleep patterns.
Causes
Bacterial causes
- Most tonsil infections and abscesses in children are caused by the Streptococcus bacterium.
- This is the same bacterium that causes ‘Strep’ throat.
- Strep tonsillitis can have serious complications and should be treated as soon as possible: it can result in the development of rheumatic fever, which can damage the heart valves; and glomerulonephritis, which can damage the kidneys. Both conditions can be fatal.
- Other complications of streptococcus infection can include scarlet fever, sinusitis, pneumonia, and ear infections.
Viral causes
- The viruses that cause the common cold or influenza (flu) may be responsible for tonsillitis.
- Rapid enlargement of the tonsils can result from a throat infection called infectious mononucleosis (glandular fever).
- The Epstein-Barr virus causes this condition.
- It also affects the adenoids and lymph nodes of the neck.
- In young children, mononucleosis is usually mild, and can be mistaken for a common cold or flu.
- When infectious mononucleosis occurs after childhood the disease can be extremely serious. It may affect the liver and spleen, and may lead to jaundice.
Symptoms
Acute tonsillitis
The typical symptoms of acute tonsillitis are a very sore throat with bright red, swollen tonsils. The onset of pain may be rapid or gradual. These symptoms may be accompanied by any of the following:
- A greyish-white discharge or spots on the tonsils
- Drooling and difficulty swallowing saliva
- Ear pain when swallowing
- Bad breath
- Swollen and tender lymph nodes in the neck under the jaw
- Fever
- Headache
- Repeated infection may cause the formation of small depressions, called crypts, on the surface of the tonsils.
- These crypts can harbour bacteria, and may contain pus pockets.
- Often, small stones called tonsilloliths are found in these crypts. These stones may contain high quantities of sulphur, and give off a characteristic "rotten egg" smell when crushed. This contributes to the patient’s bad breath.
- Tonsilloliths may also give a patient the unpleasant sensation of having something caught in the back of the throat.
Tonsillar abscess (Quinsy's abscess)
In addition to inflamed tonsils, a tonsillar abscess can result in:
- Severe pain and tenderness around the area of the soft palate, at the roof of the mouth
- Difficulty swallowing
- Muffled speech caused by swelling from the abscess
- An inability to open the mouth (trismus)
Hypertrophic tonsils (enlarged tonsils)
Enlarged tonsils and adenoids can obstruct breathing. This can result in:
- Snoring
- Disturbed sleep patterns, including:
- Sleep apnoea (when the child stops breathing for brief periods while asleep)
- Frequent awakening from sleep
- Restless sleep
- Nightmares
- Bed wetting
Such sleep-related problems can lead to the development of mood changes, excessive sleepiness, failure to thrive, and sometimes even heart problems.
- Chronic mouth breathing. This may sometimes cause the teeth to become badly aligned (malocclusion).
- Chronic enlargement and infection of the tonsils, in combination with adenoidal infection, can cause infections in other nearby structures:
- The air passages in the region of the nose may become infected (sinusitis) and problems with nasal drainage or obstruction can develop.
- The eustachian tube of the ear may also be affected, resulting in chronic ear infections.
Prevalence
Tonsillitis is a very widespread condition in young children between the ages of one and seven. It is uncommon under the age of one year. It is also uncommon in adults.
When to see a doctor
You should seek professional medical attention if:
- A child has symptoms of acute tonsillitis, as listed above.
- In addition to tonsillitis symptoms, the child begins drooling or experiences trouble breathing. This may be a sign of a tonsillar abscess.
- The child breathes with difficulty at night, or breathes noisily. This can indicate large, overgrown (hypertrophic) tonsils and adenoids.
- The child has episodes of sleep apnoea.
- The child has fever or pain that is not helped by taking antibiotics, and the tonsils have greyish-white spots or a discharge. These may be signs of mononucleosis or some other viral infection.
Diagnosis
You can easily check someone's tonsils for tonsillitis at home using the following method: Use a spoon and a torch. Depress the tongue gently with the handle of the spoon. Ask the patient to say "aaahhh" while you shine the torch onto the back of the throat. You will easily be able to see if the tonsils look bright red and swollen. If so, you should see a healthcare professional for an examination and diagnosis.
‘Strep’ tonsillitis
To diagnose a Streptococcus infection, your doctor may do a so-called rapid strep test. This test takes only about 15 to 20 minutes, and can usually be done in the doctor’s office. If the result is not strongly negative and you have strep symptoms, your doctor may then also do a more traditional throat culture, which takes longer to be analysed. Taking a throat culture is a painless procedure; it involves taking a sample of throat mucus with a swab. If your doctor’s office is not suitably equipped, the sample may have to be sent to an outside laboratory for analysis.
Infectious Mononucleosis (Glandular fever)
Because infectious mononucleosis has such a wide range of symptoms, it can be difficult for a doctor to immediately diagnose this condition. After doing a physical exam, the doctor may take a blood sample to check for the presence of abnormal white blood cells or antibodies that are diagnostic of infectious mononucleosis.
Other conditions
The doctor will also examine the tonsils and soft palate to check for the presence of a tonsillar abscess.
Treatment
- Antibiotics cannot help in the case of a viral infection. Viral infections of the tonsils are therefore often treated only with supportive care – by making sure the patient gets bed-rest, is well hydrated, and that the fever is controlled.
- A peri tonsillar abscess should be carefully drained. This can be done by removing the fluid with a needle and syringe - a procedure called needle aspiration. The abscess can also be cut open with a scalpel to drain the fluid.
- Chronic stones (tonsilloliths) in the tonsil crypts can be removed with a blunt probe, ear-bud or even with a finger (if it is clean!)
Medication
- Bacterial infections of the tonsils (such as strep throat) can be effectively treated with antibiotics, for example penicillin or erythromycin. A doctor will prescribe an appropriate course of medication for acute tonsillitis or for an abscess.
- Hypertrophic tonsils that are large enough to obstruct the airway can be treated with a long course of antibiotics. A short course of steroids can also be effective. (Steroids are cortisone-related medications, for example prednisone and prednisolone.) However, surgical removal remains the treatment of choice for this condition.
- A mild painkiller such as paracetamol may be useful to ease the pain of tonsillitis. (CAUTION: do not give aspirin to a child. Aspirin has been linked to Reye's syndrome, a rare but serious condition.)
As with any antibiotics, once treatment begins, it is important to take the full prescribed course of medication. Discontinuing the antibiotics before the end of the course, even if the patient feels better, can result in regrowth of the bacteria.
Surgery
The surgical procedure to remove the tonsils is called a tonsillectomy.
- A tonsillectomy patient may need to be hospitalised for up to 24 hours. The throat will be sore for four or five days after the operation in children.
- The removal of the tonsils does not appear to have any adverse effect on children’s immunity to infection.
When is a tonsillectomy recommended?
In the past, tonsillectomies were performed far more frequently than they are now. These days, the trend is for doctors to only recommend surgery in cases where:
- The tonsillitis is severe and resistant to medication.
- The infection is recurrent and persistent.
- The infection interferes significantly with everyday activities.
- Bad breath or tonsillar stones cause significant discomfort.
- There are serious complications as a result of infection or a high risk of such complications. These include tonsillar abscess, serious streptococcal complications (such as rheumatic heart disease or nephritis), or neck abscess.
- The tonsils are so greatly enlarged that they cause severe sleep problems (such as snoring and sleep apnoea), dental abnormalities, or difficulty swallowing.
- The tonsil infection is accompanied by adenoid enlargement, causing recurrent ear infections, nasal obstruction, or sinusitis; and where these symptoms are resistant to medication.
- There is reason to suspect the presence of a malignancy or tumour.
Prevention
In the past, the tonsils and adenoids were frequently removed during childhood as a preventative measure. However, these days doctors are generally only willing to recommend surgery in serious cases, as described above. Avoid close contact with anyone having an attack of tonsillitis, so as not to be infected.
Reviewed by: Prof Eugene Weinberg, FCPaeds [SA}, FAAAAI, Paediatrics and Paediatric Allergology, Allergy Diagnostic Unit,UCT Lung Institute, September 2011




 Publications
Publications
 Partners
Partners