Summary
- Small children are most at risk for choking, when an object gets stuck in the airway.
- Encourage a choking person to cough up the obstruction if they are able.
- If coughing is ineffective, perform abdominal thrusts and back slaps on children and adults, and chest thrusts and back slaps on babies.
- Call an ambulance and start CPR if the person becomes unconscious.
- Prevent choking by encouraging calm and careful chewing of food at mealtimes, supervising small children when they eat, and keeping them away from small objects and foods that pose a choking risk.
What causes choking?
Choking happens when an object, often a piece of food, gets stuck in the airway. Young children and babies are likely to choke on food or something they have put into their mouths.
What are the symptoms and signs of choking?
A person who is choking may instinctively grab at the throat. He or she may cough and gasp, go red in the face, have difficulty speaking and get very distressed. Coughing might still be possible if there is only a partial obstruction. Complete obstruction will cause a blue, dusky face and unconsciousness.
A choking baby may attempt to cry, make strange sounds or none at all.
First aid for choking
- If the person is coughing, encourage him or her to keep doing this. Don't interfere - they should be able to cough up the object.
- If the person cannot speak, or only has a weak cough, follow the instructions below.
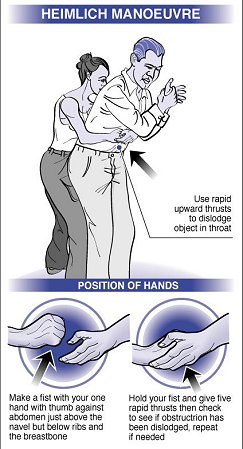
Conscious adult (9 years and older) - abdominal thrusts (Heimlich manoeuvre):
- If the person only has a weak cough, and indicates by nodding they are choking, give up to 5 abdominal thrusts, followed by 5 firm slaps with the heel of your hand, between the shoulder blades. The person needs to be leaning forward for the back slaps. Check whether the object has dislodged.
- Abdominal thrusts (Heimlich manoeuvre):
- Stand behind the person with your foot between his feet.
- Reach around the waist. Make a fist (thumb outside fingers) and use the knuckle of the thumb in the navel as a landmark. The flat part of the thumb is placed against the abdomen just above the navel.
- Grab your fist with the other hand. Keeping your arms off the person's rib cage, give 5 quick inwards and upwards thrusts. This might cause the object to pop out. Check the mouth.
- Repeat the procedure of 5 abdominal thrusts and 5 back slaps until the object is dislodged or medical help arrives. If he becomes unconscious, call an ambulance and start CPR.
- Each time you open the airway during CPR, look for an object and if visible, remove.
If you are alone:
- Try to cough up the object.
- If this doesn't help, do abdominal thrusts on yourself using your fists, or lean over the back of a chair and press down forcefully.
Conscious child (1 - 8 years)
- Encourage the child to cough. If this is ineffective, stand or kneel behind him and bend him forwards; or place a small child face down across your lap with head low.
- Do abdominal thrusts followed by back slaps (as for adult).
- Repeat the procedure until the object is dislodged or medical help arrives.
- If the child becomes unconscious, call an ambulance and start CPR.
Conscious baby (under 1 year)
- Kneel down, and lay the baby facedown on your forearm or thighs, with the head lower than the trunk, and support the head with your hand. Don't cover the baby's mouth or twist the neck.
- Give 5 hard back slaps between the shoulder blades.
- Check if the object is clearly visible, then remove with a hooked finger. Don't do blind finger sweeps. (It is safe to put a finger into a baby's mouth but in adults and children, reflex action may cause them to bite.)
- If the object cannot be removed, lay the baby face upwards along your forearm or lap, with the head lower than the trunk. Place two fingers on the breastbone just below the nipple line and give 5 downward chest thrusts to a depth of 2.5 cm.
- Check the mouth again and remove the object if visible.
- Repeat the sequence of back slaps and chest thrusts. If unsuccessful, call an ambulance and start CPR.
Note: Do not perform abdominal thrusts on a baby.
Unconscious choking victim (all ages)
- Call an ambulance immediately.
- Assess the ABCs and start CPR. Each time before you start mouth-to-mouth breathing, check whether the object is visible in the mouth. Do not perform blind sweeps. Chest compressions might dislodge the object.
- Continue with CPR until the victim is breathing on his or her own or until the ambulance arrives.
If the above measures are successful, the person must still be checked at hospital if:
- Abdominal thrusts were performed as they can cause internal injuries.
- Swelling of the airway from an infection, injury or allergic reaction caused choking.
Pregnant or obese persons
- Stand behind the person and place your arms under the person's armpits around the chest.
- Place the thumb side of your fist in the centre of the chest.
- Grab your fist with your other hand and give five inward thrusts.
- Give 5 back slaps.
- Repeat the procedure until object becomes dislodged.
Prevention
- Don't talk while eating. Drink alcohol in moderation (alcohol impairs co-ordination of the muscles used for swallowing).
- Chew food properly, and be especially careful if you wear dentures.
- Supervise young children while eating. Insist that children eat sitting quietly, preferably at the table. They should never run, play or lie down with food in their mouths.
- Don't give a small child food that can break off into hard pieces.
- Don't give popcorn, nuts, hot dogs, chunks of meat and cheese, whole grapes, hard, gooey or sticky sweets, chunks of peanut butter, corn chips, raw vegetables, raisins or chewing gum, until age 4.
- Check toys for small detachable parts. Follow age recommendations on toy packages.
- Cut foods for infants and young children into pieces under 2cm. Teach them to chew well.
- Before a child begins to crawl, go down on his level and look for dangerous items. Balloons and coins pose a big choking risk. Check under furniture and between cushions for small items.
- Beware of older children's actions. Many choking accidents occur when older siblings give dangerous foods, toys or small objects to a younger child.




 Publications
Publications
 Partners
Partners