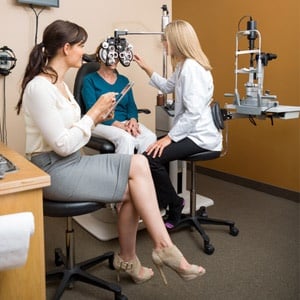
As loss of vision can be the result of some eye diseases, regular checkups are recommended every year or two for those without eye problems, and more regularly for those who have problems with their eyes.
Another reason why check-ups are important, is that many eye diseases have few or no symptoms in their early stages, but might be more difficult to treat effectively once they have become advanced. The damage caused by glaucoma, for example, is irreversible.
Read: Cataracts
There are three steps to diagnosing eye diseases according to the Merck Manuals:
• Asking the patient about the symptoms
• Looking at the appearance of the eye
• A close physical examination, which might include testing
The symptoms
Symptoms that you may be asked about by the doctor or ophthalmologist include the following, according to FamilyDoctor.org.
Tearing, blurred vision, loss of vision, injuries to the eye, the presence of floaters, redness and pain in the eye, cloudy vision, flu-like symptoms, sinus infection, sensitivity to light, possibility of being diabetic, swelling or itchiness around the eyes, painful lumps, discharges from the eye, skin irritation around the eye, and the wearing of contact lenses.
You will also be asked about your medical history and whether you have experienced this particular, or any other eye problem, before.
The appearance of the eye
Even before closely examining the eye, the doctor will be able to observe certain signs in the physical appearance of the eye. These include droopy eyelids, bloodshot appearance of the eye, an opaque appearance to the eye, a squint (strabismus), excessive tearing, trauma to the area around the eye, an inverted eyelid, swelling or bulging of certain sections of the eye, puffiness around the eye, large scratches on the cornea, inflammation of eyelash follicles and styes.
Read: Macular degeneration
Actual tests
The following tests will be done in order to diagnose your eye problem, say the Merck Manuals:
Refraction is used to assess focusing errors which can lead to visual acuity problems such as nearsightedness or farsightedness.
A person’s vision is tested by using the Snellen test - making them read letters on a chart from six metres away, or a lighted box that displays rows of letters in diminishing sizes. Read more about the Snellen test and how it works right here.
An autorefractor is also used to determine how light is changed when it enters the eye. A phoropter, used together with the Snellen test, helps to determine which corrective lenses will be most effective.
And the usage of the expression 20/20 vision? The Merck Manuals explain:
Acuity is usually measured on a scale that compares a person's vision at 20 feet (about 6 meters) with that of someone who has perfect vision. Thus, a person who has 20/20 vision sees objects that are 20 feet away with the same clarity as a person with normal vision, but a person who has 20/200 vision sees at 20 feet only as clearly as a person with perfect vision sees at 200 feet (about 61 meters).
Read: Retinopathy
Visual field testing is done to see the entire area seen out of each eye. With one eye closed, and the patient focusing on the doctor’s face, he/she moves an object into the field of vision, and makes notes on when the patient reports seeing it.
A Goldmann perimeter is used to test peripheral vision, and an Amsler grit to test the central area of vision. Eyes are always tested separately.
Isihara colour plates (coloured dots on a white background) are used to test for colour blindness. Inability to see certain patterns or numbers in amongst the coloured dots can point to colour blindness.
Ophthalmoscopy (also called funduscopy), is like a flashlight with magnifying lenses. This is used to look through the pupil into the eye using a bright light in order to detect changes in the retina or the other structures of the eye, possibly because of conditions such as diabetes or high blood pressure. An indirect opthalmascope will give the doctor a three-dimensional view.
A slit-lamp is mounted on a table and the patient rests his/her chin on a small cross bar and looks directly into this binocular microscope. A bright light is shone into the eye. This instrument allows the doctor to do a thorough examination of the structures inside and around the eye (eyelids, skin around the eyes, iris, cornea, the fluid in the front part of the eye, the lens, retina and the optic nerve).
Tonometry measures the pressure within the eye. A small puff of air is blown against the cornea. This flattens the cornea and this instrument measures how long it takes to do that. The longer it takes for the cornea to flatten, the greater the chance of the presence of certain types of glaucoma.
Read More:
Image: Optometrist team examine older woman's eyes from Shutterstock




 Publications
Publications
 Partners
Partners