Summary
- Primary open angle glaucoma (POAG) is generally a bilateral, although not symmetrical disease of the optic nerve(optic neuropathy).
- POAG causes damage to the optic nerve and, if not treated, eventually leads to blindness.
- People who are at risk for POAG include those who are over 40, diabetics, people with a family history of the condition, short-sighted people, black people, and people with heart and blood pressure problems.
- Because there are usually no symptoms until irreversible damage has occurred, regular pressure checks should be carried out on all people over age 40, especially those at increased risk of the disease.
- POAG is diagnosed by intraocular pressure assessment, examination of the optic disc and visual field measurement.
- It can be treated using eye drops, tablets, and laser or conventional surgery, but lifestyle is also an important factor.
Definition
Primary open angle glaucoma (POAG) is an optic neuropathy (disease of the optic nerve). It is generally a bilateral, although not necessarily symmetrical disease. If two or more of the following is present it is diagnosed :
- Raised intra-ocular pressure > 21mmHg
- Glaucomatous visual field defects (a test done to assess the peripheral visual field)
- Glaucomatous optic nerve damage (the part of the nerve visible in the eye becomes “cupped”. This is where the centre depressed part increases in relation to the whole disc diameter).
From this it is clear that even normal pressure can cause damage to the nerve, the so called normal lension glaucoma.
Cause
Changes occur in the outflow channels of the eye’s aqueous humor (the fluid inside the eye) in the presence of an open structured angle. This causes increased pressure in the eye and slow destruction of the optic nerve.
If the blood flow to the nerve is good, the nerve can be protected from the effects of the pressure. If the blood flow is poor in conditions such as orthostatic hypotention(low blood pressure when moving from a sitting or supine to a standing position) or heart disease.
Who gets it and who is at risk?
POAG is inherited in a multi-factorial manner
- High myopia – very short sighted people
- Increasing age
- Diabetics
- Black people
- High blood pressure problems
- Certain eye conditions like retinitis pigmentosa.
Symptoms and signs
This disease shows no symptoms until very late in the disease when extensive damage has occurred. Slow loss of peripheral vision is often not picked up by the affected person.
Cupping of the optic disc, high intra-ocular pressure and visual field defects are symptoms that may show up during medical examination ( see diagnosis below).
Diagnosis
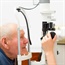
Because glaucoma may not cause any symptoms until irreversible damage has occurred, every routine eye examination – and ideally every physical examination – in all adult patients should include checking the pressure in the eye. This is called tonometry. A single normal reading does not rule out glaucoma since the eye pressure varies according to the time of day and the pressure rise in early glaucoma may be intermittent.
In addition the optic disc is examined for characteristic changes. The optic disc may appear normal or show what is called "cupping", in which the centre is depressed, indicating glaucoma. The visual fields may also be checked, and may show characteristic defects in the periphery. If glaucoma is suspected, you should have a complete assessment and frequent follow-up examinations by a specialist eye doctor (ophthalmologist) and a detailed visual field examination.
Prevention
The disease itself cannot be prevented. However, damage to the eye from the disease can be prevented if it is diagnosed early and treated correctly. Therefore all people who are at increased risk for the disease require regular eye examinations.
Treatment
Most people can be treated with drugs administered as eye drops. Each patient must be carefully assessed to determine which drugs are appropriate.
Eyedrops in use include:
- Alpha agonists: e.g. Brimonidine
- Beta blockers: e.g. Betaxolol, Levobunalol, Metipranol, Timolol and others
- Carbonic anhydrase inhibotors: e.g. Dorzolamide
- Prostaglandin agonists: e.g. Latanoprost, Travoprost and Bimatoprost
- Combinations of the above
If eyedrops fail to stop the progression of the glaucoma, then laser or conventional surgery, or oral medication (acetazolamide) is used. Laser trabeculoplasty or filtering surgery improves aqueous drainage and acetazolamide reduces production of aqueous fluid. This reduces the pressure in the eye and prevents further damage to the optic nerve and vision.
Regular physical exercise reduces intraocular pressure and protects the optic nerve, therefore this is an excellent way of additional treatment to the eye.
Outcome
Untreated, the condition leads to blindness.
Treated, vision may be preserved as long as the treatment is continued for life.
When to call the doctor
If you have any of the risk factors for this disease you should see a doctor or an optometrist at least every year for a glaucoma check. If you have glaucoma, the condition must be managed by an ophthalmologist for the rest of your life.
Previously reviewed by Dr L.C. Boezaart, M.B.Ch.B, M.Prax.Med, M.Med (Ophth), December 2004
Reviewed by Dr L.Venter, MB Ch B, MMed (Ophth) + FC Ophth SA , December 2010




 Publications
Publications
 Partners
Partners