Summary
- Ulcerative colitis is an inflammatory bowel disease.
- It causes inflammation and ulcers in the lining of the large intestine
- The exact cause is not known
- Most sufferers are between the ages of 15 and 40 years
- The most common symptoms are abdominal pain and bloody diarrhoea
- Although it is treatable there is no specific cure
- Diagnosis includes a physical exam and series of blood tests
- Adequately managed by experienced clinicians, the condition does not result in significant reduction in life-expectancy of the affected person.
Definition
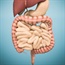
The disease causes inflammation and ulcers in the lining of the large intestine. Usually, this inflammation occurs in the rectum and lower part of the colon, but it could affect the entire colon. Due to the inflammation, the colon empties frequently, causing diarrhoea. The ulcers form in places where the inflammation has destroyed colon lining cells and they bleed and produce pus and mucus.
Ulcerative colitis is an inflammatory bowel disease (IBD), which is the collective name for non-infectious diseases that cause inflammation in the intestines. It can be difficult to diagnose because the symptoms are similar to other intestinal disorders such as irritable bowel syndrome and Crohn's disease. Crohn's disease is different from ulcerative colitis in that it causes inflammation deeper within the intestinal wall, and also frequently involves the small bowel.
Cause
Theories about what causes the disease abound, but none have been proven. The most popular theory is that the immune system reacts inappropriately to agents, such as food components, viruses or bacteria within the bowel lumen, causing ongoing inflammation in the intestinal wall. Sufferers of ulcerative colitis have abnormalities of the immune system, but doctors are unable to determine whether these abnormalities are the cause or the result of the disease. Ulcerative colitis is not caused by emotional distress or sensitivity to certain foods or food products, although these could trigger the symptoms.
It is possible that affected people have an abnormal defense mechanism against the bacteria which are normally present in the gut. A long-term reaction to a particular bacterium or virus could be significant.
Who gets it and who is at risk?
Most sufferers of ulcerative colitis are between the ages 15 to 40, although children and older people can also develop the disease too. Men and women are equally affected and the disease seems to run in some families.
Symptoms and signs
The most common symptoms are abdominal pain and bloody diarrhoea. Sufferers may also experience the following:
- fatigue and a general feeling of tiredness
- weight loss
- loss of appetite
- rectal bleeding
- loss of body fluids and nutrients
- frequent and urgent need to pass blood and mucus, there may be some stool as well
- diarrhoea in more severe cases
- abdominal pain, often just before a stool is passed
About half of the sufferers of ulcerative colitis only have mild symptoms. Others suffer frequent fever, bloody diarrhoea, nausea and severe abdominal cramps. The disease could also cause problems such as arthritis, inflammation of the eye, liver disease (fatty liver, hepatitis, cirrhosis, and primary sclerosing cholangitis), osteoporosis, skin rashes, anaemia, and kidney stones. No one knows for sure why problems occur outside the colon. Scientists believe these complications occur when the immune system triggers inflammation in other parts of the body. But these problems are usually mild and may improve if the colitis is treated properly.
Although treatable, there is no specific cure for the disease, and the condition can cause problems on and off throughout the life of the sufferer. For the best part, someone with the disease will feel fine and not suffer any of the symptoms. Then the disease would be in remission. But it flares up from time to time and becomes active – which is the relapse. With each flare-up the symptoms can be better, worse or similar to the previous bout. Adequately managed by experienced clinicians, the condition does not result in significant reduction in life-expectancy of the affected person.
Diagnosis
A thorough physical exam and a series of tests are necessary to diagnose ulcerative colitis. Blood tests could be done to check for anaemia, which could indicate that there is bleeding in the colon or rectum. Blood tests may also uncover a high white blood cell count, which is a sign of inflammation somewhere in the body. By testing a stool sample, doctors can tell whether there is bleeding or infection in the colon or rectum.
A colonoscopy could also be called for. This is when a doctor inserts an endoscope (a long, flexible, lighted tube connected to a computer and TV monitor) into the anus to see the inside of the colon and rectum.
The doctor will be able to detect any inflammation, bleeding or ulcers on the colon wall. A biopsy could then also be done, which involves taking a sample of tissue from the lining of the colon to view under a microscope. A barium enema X-ray of the colon could be required and involves filling the colon with barium, a chalky white solution. The barium shows up white on X-ray film, giving the doctor a clear view of the colon, and of any ulcers or abnormalities that might be present.
Treatment
Treatment depends on how serious the condition is but most people are treated with medication. Severe cases could call for surgery in which the entire colon would be removed. That is also the only cure for ulcerative colitis.
Management of ulcerative colitis involves treatment of the active flares of the disease, as well as attempting to ensure that the disease then remains in remission.
Steroids (cortisol) are the mainstay of treatment of active disease, and dependent on the extent and severity of disease, may be given orally, rectally (enema) or as an intravenous injection. Side effects of steroids include weight gain, acne, facial hair, hypertension, mood swings, and increased risk of infection, which is why doctors are cautious when patients take these drugs, and use them only when necessary.
Thinning of the bones (osteopenia/osteoporosis) is often associated with inflammatory bowel disease. This complication is particularly aggravated by the long-term use of steroids.
The symptoms could occasionally be so severe that the patient may need hospitalisation. This would include severe bleeding, and/or diarrhoea causing dehydration.
Once the disease is in remission, maintenance therapy is usually given with drugs such as sulphasalazine, asacol or pentasa. Asacol is also available as a suppository as well as an enema for those patients in whom the disease is limited to the end of the colon (the rectum and sigmoid colon). Possible side effects of these drugs include nausea, vomiting, heartburn, diarrhoea, and headache.
New drugs for inflammatory bowel disease, which have more targeted effects on the immune system, are currently undergoing clinical trials.
In certain cases, the symptoms may be triggered by certain foods. If the person is able to identify these foods, avoidance may assist the management of his/her condition. Milk products are the foods most often implicated, but this is by no means universal.
In view of the chronic, often unpredictable nature of this disease, regular visits to a doctor or clinic with a specialized interest in inflammatory bowel disease are strongly advised in order to monitor the condition.
Up to 40% of ulcerative colitis patients eventually have their colons removed because of bleeding, severe illness not responding to medical therapy, rupture of the colon, and/or risk of cancer.
The most appropriate surgery for ulcerative colitis is a proctocolectomy with ileo-anal pouch. A temporary ileostomy may be required prior to the final formation of ileo-anal pouch. In this operation the entire colon and rectum are first removed. A small opening is usually created in the abdomen, called a stoma (ileotomy). The end of the small intestine, called the ileum, is attached to it. Waste will travel through the small intestine and exit the body through the stoma.
The stoma is about the size of a two rand coin and is usually located in the lower right part of the abdomen. A bag is worn over the opening to collect waste, which is emptied when needed.
In order to avoid the long-term requirement of the ileostomy, an ileo-anal pouch anastomosis is usually performed. In this operation, the end of the small bowel is folded on itself to create a reservoir (pouch), and is then connected to the anus. In this way, bowel waste can be passed in the usual way, although bowel motions will be loose and rather frequent (approximately six a day). This is usually a very successful operation and is offered to most patients with ulcerative colitis who require surgery.
Outcome
Patients with ulcerative colitis do have an increased risk of developing cancer. The risk of cancer increases with the duration and the extent of the disease in the colon. If only the lower colon and rectum are involved, the risk of cancer is not higher than normal. When the whole colon is affected, the cancer risk increases dramatically, and is in the region of 5% after ten years of disease. It is therefore essential that patients with ulcerative colitis are seen by experienced physicians on a regular basis.
If they have extensive disease which has been present for more than five to seven years, they need to have their colons checked periodically (by colonoscopy) for any of the early signs of cancer. If early cancer is detected, surgery (proctocolectomy) would usually be advised.
Prevention
Not really. Since the causes are unknown the best bet would be to consult a doctor regularly if the disease runs in your family and also to seek medical advice as soon as symptoms occur.
When to call a doctor
A doctor should be consulted when there is rectal bleeding or excessive diarrhoea. There are local societies of inflammatory bowel disease patients in several of the larger centres which offer useful assistance and guidance with regard to the condition.
Reviewed by Prof T. Winter, FCP (SA)




 Publications
Publications
 Partners
Partners