Laboratory tests will aid in confirming the diagnosis of coeliac disease. Laboratory studies may show characteristic types of anaemia, as described above.
The blood may be low in albumin (a form of protein). Tests of intestinal absorption are often abnormal and there may be an abnormal amount of fat in the stool.
Certain antibody blood tests may aid in the diagnosis. An antibody known as anti-endomysial antibody is found in 95% of patients with coeliac disease and can be used to screen for the disease in relatives of affected patients or in patients suspected of having the disease.
A biopsy must be obtained to confirm the diagnosis of coeliac disease. This entails snipping off a small piece of the small intestine under guidance through an endoscopic tube (a tube that allows the doctor to see inside the body), and examining it under a microscope.
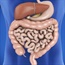
In patients with coeliac disease, the surface of the small intestine shows several highly suggestive abnormalities. Normally, the internal surface of the small intestine is covered in tiny finger-like projections called villi. These villi greatly increase the surface area of the bowel, thereby increasing the rate at which digested food particles can be absorbed into the bloodstream.
When a person has coeliac disease, these villi are destroyed so that the surface of the bowel looks flat when viewed under magnification. It is this loss of villi called villous atrophy that leads to the impairment of nutrient absorption from the small intestine.
The symptoms of the disease should improve once the patient has been placed on a gluten-free diet, and this, too, should aid in the diagnosis of the disease. A definite diagnosis of coeliac disease can be made if there is improvement of villous atrophy on repeat biopsy performed when the patient is on a gluten-free diet.
Read more:
The symptoms of coeliac disease
How coeliac disease can be treated
Reviewed by Dr Ismail Moola MBCHB (UCT) FCP (SA) Cert Gastro Phys (SA).
Specialist Physician / Gastroenterologist Netcare Sunninghill Hospital and part time Lecturer Department of Internal Medicine, Division of Gastroenterology, Wits University.
Previously reviewed by Dr G Watermeyer MBChBFCP (SA), Cert Gastroenterology (SA), Consultant GIT Clinic Groote Schuur Hospital.




 Publications
Publications
 Partners
Partners