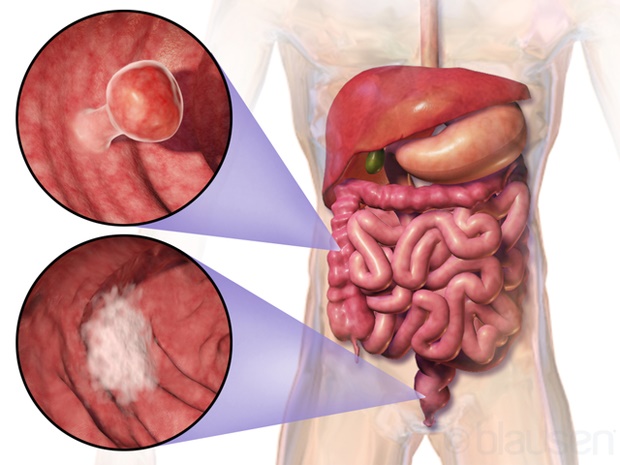
Cancer of the large bowel, colon cancer, rectum cancer. The rectum is the part of the large bowel just above the anus.
Symptoms
The doubling time of colorectal cancer is about 620 days. That means that it is a slow growing type of cancer and it may be present for as long as five years before symptoms appear.
Unfortunately, the symptoms are often so insignificant that they are ignored. The symptoms depend on where the cancer is. The more distal cancers in the rectum and the sigmoid (the part of the bowel above the rectum) may present with red blood in the stool.
Many people may think they have haemorrhoids (piles) and ignore it because the blood can come and go. When the tumour grows, it can cause bowel obstruction or grow into the pelvic bones and cause local pain.
The left side of the colon is narrower that the right, so you may have colicky abdominal pain after meals or changed bowel habits as well.
Tumours in the right colon (the caecum – where the small bowel attaches itself to the colon –, the ascending colon – the part on the right side of the abdomen – and the transverse colon – the part that is situated between the left and right side) may also cause obstruction, but often present only with anaemia, because the tumour does not bleed enough at a time for blood to be noted.
Common complaints are:
- A change in bowel habits
- Blood in the stool (red or tarry)
- Foul-smelling stool
- Abdominal discomfort such as colic, bloating or fullness
- Fatigue
- Weight loss
- A feeling that one wants to pass stool, but nothing comes out
Colorectal cancer is often misdiagnosed as irritable bowel syndrome (the so-called spastic colon), diverticular disease (balloon-like structures mostly on the left side of the colon) or haemorrhoids. It is for this reason that if you develop new abdominal symptoms, they must be fully investigated. All patients with blood in their stool should have a colonoscopy.
Image: Colorectal Cancer (By Blausen Medical Communications, Inc. - Donated via OTRS. CC BY 3.0, WikiCommons)
Take note
Colorectal cancer is one of the most common cancers that affect adults. In the United States, it is the second most common cause of cancer death in adults. The reason we must take note of this is that it’s preventable.
Most colorectal cancers develop from polyps in the colon, although not all polyps will develop into cancer. These mushroom-like growths take about 10 to 15 years to turn into cancer, and they can be detected by looking at the inside of the colon. The procedure is called a colonoscopy.
Risk factors
The risk of becoming a colorectal cancer victim starts at the age of 40. In the general population, 90% of colorectal cancers will occur in people aged 50 years and older. According to international guidelines, one should have a colonoscopy at the age of 50 and after that every 10 years. Polyps in the colon are common, especially after the age of 50, and the risk of developing cancer from polyps larger than 1 cm is 37%.
About 30% of all colorectal cancers are inherited. Family members of a patient with colorectal cancer should start with screening colonoscopies 10 years before the age their family was when cancer was diagnosed or at the age of 40 – whichever comes first. For instance, if your father was diagnosed at 40, you and your siblings should all be screened from 30 years onwards.
Some inherited forms of colorectal cancer need earlier surveillance colonoscopies. One of these conditions is called familial adenomatous polyposis, where thousands of polyps develop in the large bowel. Most people with this condition will die before the age of 40 if they are not screened from about 10 to 12 years of age and treated in the correct way. Another situation is when many family members have various forms of cancer, such as ovarian, stomach, pancreas, urinary tract and small bowel cancers. Their screening should start at the age of 20 to 25 years and be repeated every 1 to 2 years.
Another group at risk for colorectal cancer is family members of people with inflammatory bowel disease, such as Crohn’s disease or ulcerative colitis. Patients with these diseases are also more prone to develop colorectal cancer due to the chronic inflammation.
Diagnosis
Colonoscopy: in South Africa a colonoscopy is probably the most cost-effective way to evaluate the colon, as it allows the gastroenterologist to obtain tissue while doing the diagnostic procedure. A colonoscopy involves passing a lighted tube through the anus into the rectum and lower colon. In this way, polyps or a cancer can be seen by the doctor.
When a polyp is found in the colon, it can be removed or small pieces can be sent to the pathologist who will report if the polyp is one of those that may develop into a cancer if left long enough. Once the doctor receives the report, he or she will decide on the next step.
Other methods to test for cancer include
- Testing for blood or genetic material such as DNA in the stool
- Capsule endoscopy: one swallows a camera the size of capsule that take pictures at a very fast rate
- CT colonography: the radiologist constructs a 3D image of the bowel. Patients receive quite a large dose of radiation with this procedure, but it is non-invasive.
- The CD 24 blood test: this is a new test that will be positive in over 90% if a cancer is present, and over 80% when a significant polyp is present.
- Genetic testing is also available for conditions such as familial adenomatous polyposis (see above).
Prevention
The cornerstones of colorectal prevention are screening and detection of polyps. We can also try to modify our risk with lifestyle, dietary changes, physical activity and medication.
Physical activity
Moderate physical activity (such as brisk walking 3-4 hours per week) can reduce your risk of colorectal cancer by 20-30%. The reason for this is not clear, but could be because exercising reduces insulin levels, abdominal fat and systemic inflammation.
Diet
Fruit, vegetables and fibre
For about 40 years it was believed that a diet high in fibre, especially from fruit and vegetables, lowered the risk of colorectal cancer. However, recent large case-controlled studies showed a nonexistent or weak association between fibre intake and colon cancer. Furthermore, no association was found between specific subtypes of fibre (including fibre from cereal, fruit or vegetables) and cancer location or stage.
However, in a study that included more than 700 000 people, it was concluded people who naturally eat a high-fibre diet, also follow a generally healthy lifestyle and have other protective factors that reduce their cancer risk. They consume other nutrients with anti-cancer effects, such as folate. In these studies, ispaghula husk (a type of fibre used in laxatives) was unexpectedly associated with an increased risk of polyp formation.
Finally, it was thought that resistant starch (starches that take a long time to digest, as in lentils, beans, etc.) might also have anti-cancer properties, but doses of 30 g per day failed to reduce the risk in studies done over four years. This dose was also three times higher than typical intake, making it an impractical diet to follow.
Red meat, fat and carbohydrates
In the past, it was believed that there was an association between red and processed meat and colorectal cancer. Men who ate pork, beef and lamb as a main meal more than five times a week, had a threefold increase in risk of colorectal cancer. But today we know that the culprit is not the meat, but the cooking process.
Several studies have found that meat eaters who consume meat with a heavily browned surface or meat that has been prepared at prolonged high temperatures, are those with the increased risk. It also seems as if gender and sex may play a role in this regard. Some women can, because of genetic factors, metabolise (acetylate) these cancerous substances rapidly and have high risk of cancer, in contrast with those who have a slow acetylation with a low risk.
Other sources of animal protein (dairy products, fish and poultry) are associated with a reduced risk of colorectal cancer and polyps.
Calcium and vitamin D
Calcium intake can reduce the risk of developing polyps and colorectal cancer, but the intake should be 700-800 mg per day. This seems to be a threshold level, and higher doses are not beneficial.
The protective effect of calcium appears to be limited to people with higher vitamin D levels. The vitamin D level (25(OH)-D) in the blood should be above 30 nmol/L. This is achieved by a daily intake of 1 00-2 000 IU per day.
Calcium and vitamin D are found in cod liver oil, milk and milk products as well as in cereals, and sun exposure helps to form vitamin D in the skin.
B vitamins
Vitamins B6 (pyridoxine) and B9 (folic acid is the synthetic form, folate is the natural vitamin) seem to play important roles in colorectal cancer. Dietary folate is much better than the synthetic folic acid found in supplements. People who benefit most from extra folate are those that have low baseline levels. Here folate can prevent the formation of polyps and cancer.
However, if you already have polyps or cancer, extra folate may aggravate the growth. Finally, it requires more that 10 years of extra folate intake before it becomes beneficial.
Although a higher intake of vitamin B6 showed a 30-40% decrease in colorectal cancer, especially in those who drink a lot of alcohol, some data suggest too much vitamin B6 could increase the risk for rectal cancer. Further studies are in the pipeline to clear up this controversy.
Antioxidants and other micronutrients
Various antioxidants have been studied to determine their role in cancer prevention, especially selenium. Beta-carotene (vitamin A) raised concerns about an increased risk for lung cancer and ischaemic heart disease in smokers. In randomised trials specifically designed to examine antioxidant supplements, no reduction in risk for colorectal cancer was found.
Western diet
It seems that a Western diet consisting of large amounts of red meat and highly refined carbohydrates is associated with an increased risk of colorectal cancer compared with a more prudent diet which includes small amounts of red meat and refined carbohydrates. The potential anticancer benefit of such dietary patterns may be related to the levels of insulin or inflammation (see later).
Lifestyle
Alcohol
Studies that included more than 500 000 participants showed that high levels of alcohol intake are associated with an increased risk for rectal more than colon cancer. The mechanism by which alcohol promotes cancer, is unknown, but it is possibly because of alcohol’s ability to reduce folate levels. The type of beverage (beer or wine) does not play a role.
Tobacco
Smoking increases the risk for colorectal cancer. The cancer forms about 30 to 40 years after the first exposure, and the risk disappears only after 31 years of cessation. The risk increases especially if you smoke more than 40 cigarettes per day, if you started smoking early in life or if you’ve been smoking for a long time.
Body mass and fat distribution
In a large study that involved more than 7 million people including about 94 000 with colorectal cancer, it was found that a body mass index (BMI, weight in kg divided by the square of height in meters) plays a definitive role in colon cancer. The increased risk was:
- BMI 23-25: 14%
- BMI 25-27: 19%
- BMI 27,5-29,9: 24%
- BMI 30 and higher: 41%
Men have a higher risk than women if their waist circumference increases.
The mechanism of how obesity increases risk for colon cancer is not well established, but it high insulin levels may be the reason. Insulin increases growth factors in the body that may promote the formation of cancer.
Medications
Aspirin, non-steroidal anti-inflammatory drugs (NSAIDs – painkillers that don’t contain steroids or paracetamol) and cox-2 selective inhibitors (painkillers that are designed to cause fewer stomach ulcers) can all reduce the risk of colon cancer. However, aspirin-related medications can cause serious bleeding from the stomach and small bowel, especially in older people, and the cox-2 inhibitors can cause a stroke or heart attack. Therefore it is not routinely used to prevent colorectal cancer.
Patients that had their colorectal cancer successfully removed, may benefit from using these medications because it reduces their mortality by 21%. It also decreases the number of polyps in patients with familial andenomatous polyposis.
Postmenopausal hormone therapy appears to be associated with a lower risk for colorectal cancer, but it is not yet clear which preparation is optimal. If hormone replacement is not started soon after the menopause commences, it may increase one’s risk for breast cancer, stroke and a heart attack.
In summary, as many as 70% of colorectal cancers can be prevented through moderate changes in lifestyle and diet.
Procedure
That will depend on where the cancer is and how far it has progressed. Most people will need an operation or stent. An operation might cure you, but if the cancer is too far advanced to be cured, an operation will still be necessary to relieve the obstruction or bleeding the cancer will cause. A stent is an expandable “spring” that can be put into the colon via a colonoscope (without an operation) and its function is also to relieve obstruction as a temporary measure. Although age and general health may play a role in the outcomes of the surgery, the tumour-associated outcome is not affected by age. Therefore, cancer surgery should not be limited or denied on the basis of age.
A colostomy (the so-called bag) is only necessary if the cancer is very low in the rectum.
For more advanced cancers, chemotherapy will be administered within eight weeks following surgery. Some patients with rectal or rectosigmoid cancer may receive radiation therapy before and after surgery.
Patients will be followed up at short intervals after the surgery and a blood test, the CEA (a tumour marker that will tell if the cancer has recurred) will be performed regularly.
Prognosis
There are many factors that influence the prognosis, such as the differentiation (how close to or far from normal tissue it looks to the pathologist), if blood vessels were involved, how deep the cancer has penetrated into the bowel, etc.
Clinical factors that influence the prognosis are one’s age (under the age of 30 is less good), if you had symptoms (no symptoms, better prognosis), if rectal bleeding was present (better prognosis), if the CEA level was high before the operation (not good), if the cancer has spread to other areas (not good), where the cancer is (better for colon than rectum, better for left-sided cancers than right-sided) and if a bowel obstruction or perforation was present (not good).
Following resection of the cancer, lifelong follow-up will be needed to detect spread locally and to other organs such as the liver. Two to three years after resection, the chances of the cancer recurring become very slim, but surveillance is still necessary as new polyps might develop.
Reviewed by Dr C R Jacobs, Clinical Oncologist, August 2008.
Reviewed by Dr Estelle Wilken, Senior Specialist, Internal Medicine and Gastroenterology, University of Stellenbosch and Tygerberg Hospital, August 2010




 Publications
Publications
 Partners
Partners