The research points ups an important message, said Dr Shelley Hwang, chief of breast surgery at Duke University Medical Centre in Durham, North Carolina. "More screening is not necessarily better. Smarter screening is better," said Hwang, author of a commentary accompanying the study. Both were published online in the journal JAMA Internal Medicine.
The study found many more women at high lifetime risk of developing breast cancer – a group advised to consider MRI – are getting the test than in years past. Those numbers rose from 9% in 2005 to 29% in 2009.
These results "suggest that breast MRI is being used better," said lead researcher Karen Wernli, an assistant investigator at the Group Health Research Institute in Seattle.
However, in a separate but related study reported in the same issue, Harvard Medical School researchers found that breast MRIs between 2000 and 2011 jumped 20-fold, then declined and stabilised by 2011. But fewer than half of women with documented genetic mutations that raise the risk of breast cancer got the highly sensitive tests, they found.
Genetic mutations
Under guidelines on use of breast MRI, the American Cancer Society and the National Comprehensive Cancer Network advise considering MRI if a woman's lifetime risk of breast cancer is greater than 20%. In the general population, a woman's lifetime risk is about 12%.
Women considered high risk are those known to have the genetic mutations BRCA1 and BRCA2, those who had chest radiation during childhood, or those with a first-degree relative known to have the BRCA1 or BRCA2 mutation, Wernli said.
For high-risk women, annual MRIs and mammograms are recommended.
More expensive than mammogram
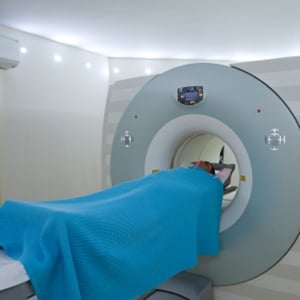
MRI uses a strong magnetic field and radio waves, not X-rays, to produce a detailed image. A scan takes about an hour. The patient lies inside a narrow tube, face down on a platform with openings so the breasts aren't compressed. Sometimes a contrast material is injected by IV to show tissue details.
The scan is more expensive than a mammogram. For instance, Medicare and Medicaid reimburse $880 to about $1 600 for MRIs of both breasts, and $300 for a digital mammogram. Fees for women not on Medicare range greatly.
Although MRIs are more sensitive in finding cancers than mammograms, false positive results are also more likely, according to research. And that can lead to unnecessary testing, anxiety and biopsies.
Wernli said she and her colleagues "wanted to see why women were getting MRIs and how these patterns changed over time." This is important to ensure that health care funds are used wisely, they said.
Dramatic increase
Her team looked at data from five national breast cancer registries from 2005 to 2011. They found the overall rate of breast MRIs nearly tripled, from about four exams for every 1000 women to almost 12, during that period. Most commonly, MRI was used to diagnose or screen for breast cancer.
In the other study, the Harvard researchers evaluated more than 10 000 women, aged 20 and older, who had at least one breast MRI. They found breast MRIs increased dramatically from 2000 to 2009, before stabilising. Most of the tests were done for screening or surveillance.
When they looked at a subset of the women who received MRIs, only 21% met the cancer society criteria.
More information
To learn more about breast MRI, visit American Cancer Society.




 Publications
Publications
 Partners
Partners











