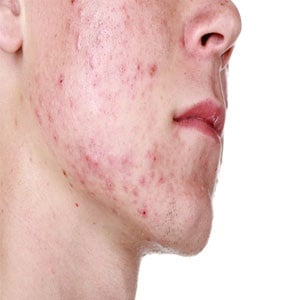
The A-Z of this medication for the treatment of acne
Isotretinoin has revolusionised the treatment of acne since it became available in South Africa in 1984, according to the National Dermatology Working Group led by Dr Dave Presbury.
It is the only treatment that affects all four aetiological factors implicated in the acne process namely:
- the production of sebum
- comedogenesis
- colonization of the skin surface and follicular duct with Propionibacterium acnes and monocyte chemotaxis with an anti-inflammatory effect.
Isotretinoin is the treatment of choice for:
- severe acne (nodulocystic acne, and extensive acne involving the face and trunk)
- lesser degrees of acne, particularly where scarring is occurring
- where other options have failed or are unsuitable or not tolerated.
Isotretinoin can also be prescribed for other conditions: Seborrhoea, Gram-negative folliculitis, Rosacea, and Hidradentis suppurativa.
More and more patients are failing to respond to long-term antibiotics, both topical creams or tablets. This is due to the increase in resistance of P.acnes to many antibiotics.
Studies have shown that even people with mild to moderate acne may develop scars for which long-term management remains a problem.
Scarring from acne may have long-term physical and emotional ramifications. Other treatments are slower in onset of action, and scarring may occur before they take effect.
Dosage and success rate
In 60 – 80 percent of people, the treatment can lead to a permanent cure at a dose between 0,5 – 1 mg/kg body weight per day for 16 – 20 weeks. New evidence suggest that a cumulative dose of 120 mg /kg body weight during the course at a daily dose of at least 0.75 mg/kg body weight may be more important than the duration of the treatment.
If acne persists or recurs a second full course may be considered any time after a two month gap following treatment.
Please note that some people – those with multiple macrocomedones and polycystic ovarian syndrome may take a while to respond to the treatment. In about 30 percent of patients, the acne becomes infected with the bacterium Staphylococcus aureus. Bacterial infections should be treated with the appropriate antibiotics. Note that tetracyclines should not be taken with isotretinoin.
With an expected 60 – 80 percent cure rate, 20 – 40 percent of people may need an extra oral antibiotics, hormonal treatment (Diane) or repeat isotretinoin.
People who might need a second course, include:
- Those with severe acne
- Those who have worsening acne before the age of 15
- Women older than 25 years at the onset of treatment
- Those with a prolonged history of acne
- Those with loads of acne on the back or trunk
- The presence of macrocomedones
- Polycystic Ovarian Syndrome
An acne flare can be anticipated in 6 percent of patients early in the course.
Possible side-effects and drug interactions
The keywords here are:
- Definitely not before or during pregnancy because it can lead to defects in the unborn baby
- Depression – patients should be counseled about possible mood changes, and if they are severe, the drug should be stopped and the patient sent for psychiatric help.
- Liver function and lipid monitoring in people with diabetes or hereditary elevated levels of triglycerides
- Not to taken with tetracycline antibiotics. The combination of tetracycline antibiotics and isotretinoin is contraindicated as each may in rare cases induce benign intracranial hypertension.
It is well known that the use of isotretinoin before and during pregnancy can impact on the development of the foetus, and can lead to congenital birth defects.
The guidelines for the use of isotretinoin in women should be observed very strictly:
- No women should take isotretinoin if she is pregnant or believes that she might be pregnant.
- Pregnancy must be avoided 4 weeks prior to, during treatment and 4 weeks after treatment has been stopped.
- Strict and reliable contraception must be used thoughout this period.
The side-effects of isotretinoin are those of excessive vitamin A. Avoid vitamin A supplement before, during and even after treatment.
Side-effects are common, but other than the potential harmful effects on the unborn child, the side-effects are uncomfortable or unpleasant rather than dangerous. Watch out for signs of depression. The drying effect is exaggerated by the dry winter climate in summer rainfall areas of South Africa.
Slight elevations of liver enzymes may occur in 10 percent of patients treated with isotretinoin. However liver problems seem to be extremely rare. Cholesterol elevation is possible, but unlikely. Monitoring of liver function and specifically of triglycerides, aspartame aminotrensferase and alanineaminotransferase.
Here is a list of potential side-effects (and their management)
Chapped lips – frequent lip balm
Dry skin and itching – avoid soap. Apply aqueous cream.
Nose bleeds – apply Vaseline several times daily to the insides of the nostrils
Dry eyes – use eye ointment
Joint and muscle pains – avoid strenuous exercise
Dry mouth – frequent fluids
Rash – emollients
Temporary hair thinning – should return to normal within a year
Photosensitivity – sunscreen, SPF 15 or higher
Headache – painkiller
Mood changes – treat depression and stop treatment
Skin fragility – do not use waxing to remove hairs
Image: acne from Shutterstock




 Publications
Publications
 Partners
Partners











