The day Evelina* – one of my favourite staff nurses – died, I realised that death sometimes puts on a shiny coat and hangs a sign stating “TB" around its neck. It takes a casual walk in the corridors of clinics and hospitals, shopping malls, churches and schools. It starts conversations with unsuspecting people and infects them, and before you know it, "death in shining armour" has killed another person.
Awareness and stigma
While writing this article, I tried to remember how many different tuberculosis awareness posters I had seen on hospital and clinic walls. I can’t remember any. Not that there weren’t any – but the posters on the walls were very bland, crowded and uninformative saying little more than that coughing, weight loss and night sweats are signs of TB. If even I, a doctor, can’t remember one example of an informative poster, how would a patient ever remember anything?
While I was working in clinical practice, patients would often say to me, “Doctor I have the flu – my nose is running, my throat hurts and I have earache.” Up to this day, I cannot recall a single patient walking into my office saying, “Doctor, I cough, I sweat at night, I have lost weight and I think I might have TB.”
You can argue that the incidence of flu is much higher than that of TB, but one would think that people would be much more aware of something that could potentially kill them, their family and colleagues.
It made me wonder if there are stigmas attached to having TB. I started to ask diagnosed patients if they were embarrassed to have TB. Only one lady felt ashamed. When I asked this woman who weighed no more than 40kg why she felt ashamed, she said, “Doctor, people think if you have TB you have Aids too, and now they think that either my husband or I sleep around.”
Read: 15 facts you need to know about tuberculosis
Protective Gear
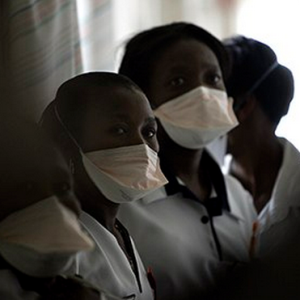
Being in the frontline of the battle against communicable diseases, one would think that government would go out of its way to protect health workers treating TB patients. This is in fact very far from the reality. Even in big academic hospitals it was often an impossible to find any of the necessary personal protective equipment like N95 masks.
N95 masks are specifically designed to protect against droplet infection of airborne agents like TB. In community health centres this was even more of a struggle. The masks that were available were often too big or too small, or so deeply hidden away that it was almost impossible to find them. More often they were just out of stock. Health workers then have to rely on normal surgical masks that are basically useless. Cost is presented as the main reason why N95 masks are not readily available.
Do we, as health workers, fail ourselves?
A colleague of mine contracted TB while she was doing her community service. The hospital where she worked had poor ventilation and was very overcrowded. When she started coughing and experiencing chest pain, she had an X-ray taken.
What is even more concerning is that occasionally even doctors lack the knowledge to treat TB. My colleague was told by her doctor that, despite a clear history and X-ray signs, he thought she had a lower respiratory tract infection.
“I think we as doctors have a denial attitude to TB”, my colleague, who wishes to remain anonymous, said. And this is the sad reality: we grow accustomed to everything we are exposed to, but often fail to recognise the signs when it affects us, as healthcare workers.
Read: Drug-resistant TB remains a crisis
Caring for others starts with you
By far one of the biggest problems I came across in clinical practice was that of patients not taking their medication. I can understand that swallowing a handful of pills every day can’t be nice, but getting daily injections if you develop resistant TB must surely be a lot worse. Fading to nothing more than a skeleton in front of your children must be so much worse than being compliant with your medication. I still can't understand why is taking one's medication is such a problem.
Evelina died because of drug resistant TB that she contracted while caring for a terminal HIV/TB patient. The patient she cared for was not compliant with his medication. He had three previous cases of TB.
Who was responsible for Evelina's death? Was the patient she cared for at fault, or can one hold the government responsible for not having the necessary protective gear available? Is it maybe because of poor awareness among the public? Or was Evelina missing the signs up to the point where it was too late.
Evelina died because she did her job. Untimely, unnecessary and preventable. How can we stop this?
*Not her real name
Read more:
Incorrect medication worsens drug-resistant TB




 Publications
Publications
 Partners
Partners










